Description
Comprehensive Diagnostic Approach and Differential Diagnosis of Arterial Hypertension: A Clinical Reference
Arterial hypertension is a pervasive and complex clinical condition that stands as a primary driver of global cardiovascular morbidity and mortality. It is fundamentally defined by a persistent elevation of systemic arterial blood pressure, which, if left unaddressed, results in a cascade of structural and functional alterations across multiple organ systems. Often termed the “silent killer,” the pathology frequently progresses without overt symptoms, making the diagnostic approach—a systematic and multi-staged process—the most critical element in preventing catastrophic outcomes such as myocardial infarction, cerebrovascular accidents, and end-stage renal failure. The diagnostic challenge for the clinician lies not only in the accurate measurement and classification of blood pressure but in the sophisticated task of differentiating primary (essential) hypertension from the myriad of secondary (symptomatic) etiologies, each of which requires a distinct and often highly specific investigative logic.
Physiological Foundations and Pathophysiology of Blood Pressure Control
To understand the diagnostic nuances of hypertension, one must first consider the complex and incompletely understood mechanisms that govern blood flow and arterial pressure. At its most fundamental level, arterial blood pressure ($BP$) is the product of cardiac output ($CO$) and total peripheral resistance ($TPR$), expressed by the formula $BP = CO \times TPR$. This balance is maintained by a highly integrated renal-volume-endocrine pressure control system.
Hemodynamic Determinants
The regulation of cardiac output is primarily influenced by stroke volume—which depends on myocardial contractility and the volume of the intravascular compartment—and heart rate. Simultaneously, peripheral resistance is determined by functional and anatomic changes in the small arteries and arterioles. In the hypertensive state, the Mosaic Theory of Hypertension, first proposed in the 1940s and refined in recent years, suggests that the condition is the result of many interdependent nodes—including oxidative stress, inflammation, sodium homeostasis, and the microbiome—that interact to raise blood pressure and cause end-organ damage.
The Renal-Endocrine Axis
The kidneys play a central role in long-term blood pressure control through the regulation of sodium handling and the activation of the renin-angiotensin-aldosterone system (RAAS). When renal perfusion decreases or sodium delivery to the macula densa is reduced, the juxtaglomerular apparatus releases renin. Renin cleaves angiotensinogen to produce angiotensin I, which is then converted by the angiotensin-converting enzyme (ACE) into angiotensin II—a potent vasoconstrictor that also stimulates the adrenal cortex to release aldosterone. Aldosterone promotes sodium and water retention in the distal nephron, thereby increasing intravascular volume. Disruptions in this axis, whether through primary adrenal pathology or secondary renal artery stenosis, are hallmark features of symptomatic hypertension.
Taxonomy and Classification of Arterial Hypertension
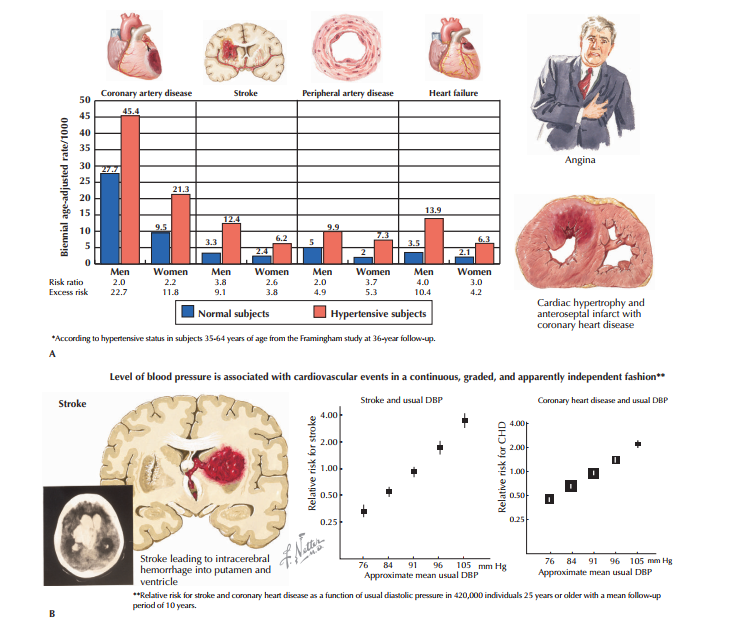
The classification of hypertension has evolved significantly, shifting from rigid thresholds to a risk-based continuum. Current guidelines emphasize that the risk of cardiovascular disease (CVD) begins to double with each increment of $20$ $mmHg$ in systolic blood pressure or $10$ $mmHg$ in diastolic blood pressure across the range from $115/75$ to $185/115$ $mmHg$.
Standard and Historical Classifications
The definition of hypertension traditionally rests on recommendations from the American Joint National Committee (JNC), the British Society of Hypertension, and the European Society of Hypertension. While slight differences exist, the core classification remains centered on office-based measurements.
| Category | Systolic BP (mmHg) | Diastolic BP (mmHg) |
| Optimal | $<120$ | $<80$ |
| Normal | $120-129$ | $80-84$ |
| High Normal | $130-139$ | $85-89$ |
| Stage 1 Hypertension | $140-159$ | $90-99$ |
| Stage 2 Hypertension | $160-179$ | $100-109$ |
| Stage 3 Hypertension | $\geq 180$ | $\geq 110$ |
| Isolated Systolic Hypertension | $\geq 140$ | $<90$ |
Isolated systolic hypertension is particularly common in older populations and is defined by an elevated systolic pressure with a normal diastolic value (usually $<90$ $mmHg$ in European guidelines or $<80$ $mmHg$ in some American standards).
The 2024 ESC Simplification
In a landmark shift, the 2024 European Society of Cardiology (ESC) guidelines introduced a simplified categorization to facilitate early intervention and clearer risk stratification. This framework replaces the “Optimal/Normal/High Normal” tiers with a more direct approach.
- Non-elevated Blood Pressure: Systolic BP $<120$ $mmHg$ and diastolic BP $<70$ $mmHg$.
- Elevated Blood Pressure: Office systolic BP of $120-139$ $mmHg$ or diastolic BP of $70-89$ $mmHg$. This category highlights individuals who, while not reaching the traditional $140/90$ $mmHg$ threshold, already exhibit an increased cardiovascular risk profile.
- Hypertension: Confirmed office systolic BP $\geq 140$ $mmHg$ or diastolic BP $\geq 90$ $mmHg$.
Furthermore, the clinical stages of hypertension are now increasingly defined by the presence of hypertension-mediated organ damage (HMOD) or comorbid conditions. Stage 1 is generally uncomplicated, Stage 2 involves the presence of HMOD, diabetes, or CKD stage 3, and Stage 3 is reserved for patients with established cardiovascular disease or advanced renal failure.
Clinical Picture and Presentation Across the Life Span
The clinical presentation of hypertension is highly heterogeneous, influenced by the age of the patient, the duration of the elevation, and the underlying etiology. While many patients are entirely asymptomatic, specific age groups present with unique diagnostic challenges and characteristic findings.
Neonatal Hypertension
In neonates, hypertension is defined statistically, with blood pressure values at or above the $95th$ percentile for post-conceptual age on three separate occasions. Recognition is often challenging as it is frequently discovered during the management of other neonatal complications.
- Clinical Presentation: Neonates may exhibit non-specific signs such as poor feeding, irritability, lethargy, or respiratory distress. In severe cases, they may present with heart failure or cardiogenic shock.
- Unique Etiologies: The use of umbilical artery catheters is a primary risk factor, as it can lead to endothelial injury and thrombus formation in the renal vessels, triggering the RAAS. Other causes include bronchopulmonary dysplasia (BPD), patent ductus arteriosus (PDA), and congenital renal anomalies such as autosomal recessive polycystic kidney disease (ARPKD).
Childhood and Adolescence
Hypertension in the pediatric population (ages 1–17) is categorized using normative distributions based on gender, age, and height. Primary hypertension is increasingly common in this group, primarily due to the global rise in childhood obesity and sedentary lifestyles.
- Small Children (<12 years): Hypertension in this group is more likely to be secondary, with renal parenchymal disease being the leading cause. Symptoms are rare, but severe cases may present with vomiting, seizures, or growth retardation.
- Adolescents ($\geq$ 13 years): The diagnostic thresholds align more closely with adult values ($130/80$ $mmHg$ for Stage 1). Primary hypertension often clusters with other risk factors like hyperlipidemia or insulin resistance. These patients may report exertional headaches or palpitations, but the majority are identified during annual wellness screenings.
Hypertension in Pregnancy
Hypertension in pregnancy remains a leading cause of maternal and fetal morbidity. It is classified into chronic hypertension, gestational hypertension, and pre-eclampsia.
- Clinical Features: Gestational hypertension is defined as new-onset hypertension after $20$ weeks of gestation. Pre-eclampsia, a more severe manifestation, involves the addition of maternal organ dysfunction, such as acute kidney injury (creatinine $\geq 90$ $\mu mol/L$), liver involvement (elevated AST/ALT), or neurological symptoms.
- Risk Indicators: Patients may present with rapid-onset edema, severe occipital headaches, visual disturbances (scotomata), and epigastric pain. These symptoms signal a transition toward eclampsia, a life-threatening state of hypertensive encephalopathy in the pregnant patient.
Middle-Aged and Elderly Adults
In middle-aged adults, primary hypertension accounts for $85-95\%$ of cases and is often associated with the metabolic syndrome—obesity, insulin resistance, and dyslipidemia.
- Elderly with New-Onset Hypertension: This demographic often presents with Isolated Systolic Hypertension (ISH), driven by the progressive loss of arterial elasticity and the stiffening of large conduit vessels. The widening of the pulse pressure (systolic minus diastolic) is a hallmark of this process and a potent predictor of stroke and heart failure.
- Secondary Suspicion: The sudden development of hypertension in a patient over $55$ who was previously normotensive should raise immediate suspicion for atherosclerotic renal artery stenosis.
Hypertension-Mediated Organ Damage (HMOD)
The consequences of sustained high blood pressure are manifested through Target Organ Damage. These complications are summarized here as essential diagnostic markers :
- Cardiovascular: Left ventricular hypertrophy (LVH), coronary artery disease, myocardial infarction, and heart failure (decompensated, orthopnea, and paroxysmal nocturnal dyspnea).
- Cerebrovascular: Transient ischemic attacks (TIA), ischemic or hemorrhagic stroke, and vascular dementia.
- Renal: Proteinuria, microalbuminuria, and progressive decrease in GFR leading to chronic renal failure.
- Retinal: Hypertensive retinopathy, ranging from arteriolar narrowing and AV nipping (Grade I/II) to cotton wool spots, flame hemorrhages (Grade III), and papilledema (Grade IV).
- Peripheral Vascular: Claudication and peripheral arterial disease (PAD).
The Diagnostic Pathway: Step-by-Step Clinical Approach
The diagnostic journey begins with the confirmation of elevated blood pressure and progresses through a structured evaluation of risk factors, HMOD, and the exclusion of secondary causes.
Verification and Measurement Technique
Inaccurate measurement is the most common cause of “pseudo-hypertension.” Diagnostic protocols require that the patient be seated quietly for at least $5$ minutes with the arm at heart level. Cuffs must be appropriately sized—a small bladder relative to the arm circumference will cause a false elevation.
| Measurement Method | Diagnostic Utility and Logic |
| Office BP | Standard screening; requires $\geq 3$ sets of readings at weekly intervals for confirmation. |
| HBPM (Home) | Identifies “white-coat” hypertension; requires twice-daily readings for $3-7$ days. |
| ABPM (Ambulatory) | Gold standard for 24-hour control and nocturnal “dipping” status; essential for patients with sleep apnea or CKD. |
For patients with atrial fibrillation, manual auscultation is mandatory, as automated oscillometric devices often fail to accurately detect mean arterial pressure in the presence of irregular heart rhythms.
The Initial Screening Panel
Every newly diagnosed hypertensive patient requires a baseline evaluation to assess global risk and screen for obvious secondary markers. This includes :
- Biochemistry: Serum electrolytes (potassium is crucial), urea, creatinine, and fasting blood glucose.
- Lipids: Total cholesterol, HDL, LDL, and triglycerides.
- Urinalysis: Dipstick for protein, glucose, and microscopic examination for casts or hematuria.
- Electrocardiogram (12-lead): Screening for LVH (Sokolow-Lyon index) or evidence of prior myocardial ischemia.
Differential Diagnosis: Essential vs. Secondary Hypertension
The clinical differentiation between primary (essential) and secondary (symptomatic) hypertension is a pivotal decision point. Primary hypertension is a diagnosis of exclusion, yet it constitutes the vast majority of cases. Clinicians must apply a “High Index of Suspicion” for secondary causes in specific scenarios.
Indications for Secondary Workup
A comprehensive evaluation for a secondary cause is warranted when:
- Hypertension develops before age $40$ (except in obese young adults, where OSA screening is the first step).
- The onset is abrupt or there is rapid worsening of previously stable blood pressure.
- Hypertension is resistant to three drugs, including a diuretic.
- There are severe elevations ($\geq 180/110$ $mmHg$) or hypertensive emergencies.
- Specific clinical clues or abnormal baseline tests are present (e.g., unprovoked hypokalemia or an abdominal bruit).
The “ABCDE” Diagnostic Logic
A structured mnemonic assists in the prioritization of secondary causes during the diagnostic encounter :
- Accuracy of diagnosis, Apnea (OSA), and Aldosteronism.
- Bruits (Renovascular) and Bad kidneys (Parenchymal).
- Catecholamines (Pheochromocytoma), Coarctation, and Cushing’s.
- Drugs (NSAIDs, OCPs, illicit substances) and Diet (excessive sodium or alcohol).
- Endocrine (Thyroid/Parathyroid).
Exhaustive Investigation of Secondary Hypertensive Etiologies
The logic for differentiating specific secondary types relies on a synthesis of history, physical examination, and targeted biochemical or radiological testing.
Renal Parenchymal and Renovascular Hypertension
Renal causes are the most frequent secondary etiologies and must be ruled out through a systematic analysis of renal function and anatomy.
- Renal Parenchymal Disease: Conditions such as glomerulonephritis, polycystic kidney disease, and chronic pyelonephritis cause hypertension through sodium retention and RAAS activation.
- Logic: Look for proteinuria, hematuria, or casts in urinalysis. Ultrasound will reveal small, shrunken kidneys in chronic failure or enlarged, cyst-filled kidneys in PKD.
- Renovascular Hypertension (Renal Artery Stenosis): This is caused by fibromuscular dysplasia (younger women) or atherosclerosis (older patients).
- Logic: Suspect when hypertension is resistant or if a systolic-diastolic bruit is heard over the abdomen. The first test is Duplex ultrasound, followed by CT or MR angiography. Renal angiogram remains the “gold standard” for definitive diagnosis.
Primary Aldosteronism (Conn’s Syndrome)
Primary aldosteronism is the autonomous overproduction of aldosterone, leading to sodium retention and potassium wasting. It is far more common than previously thought, and the 2024 ESC guidelines now recommend screening for it in all adults with confirmed hypertension (Class IIa).
- Diagnostic Path: The initial screening test is the Plasma Aldosterone Concentration to Plasma Renin Activity (PAC/PRA) ratio (ARR). An elevated ratio (typically $>30$) is highly suggestive.
- Diversification: Confirmation requires a suppression test (saline infusion or oral salt loading) to demonstrate the failure of aldosterone to decrease. Localization of an adrenal adenoma vs. bilateral hyperplasia is then performed via CT/MRI or adrenal venous sampling—the latter being the only definitive way to distinguish unilateral from bilateral disease.
Pheochromocytoma and Paraganglioma
These are catecholamine-secreting neuroendocrine tumors. Although rare, they are critical to diagnose due to the risk of lethal hypertensive crises.
- Clinical Clues: Paroxysmal hypertension associated with the classic triad of headache, palpitations, and diaphoresis. Other signs include orthostatic hypotension and impaired glucose tolerance.
- Logic: The first-line test is the measurement of plasma or 24-hour urinary fractionated metanephrines. High sensitivity makes a negative test effective for ruling out the condition. Localization is achieved through CT or MRI of the abdomen and pelvis; 18F-FDOPA PET-CT is useful for metastatic or extra-adrenal sites.
Cushing’s Syndrome
Hypertension occurs in $80\%$ of patients with Cushing’s syndrome, where excess cortisol increases vascular sensitivity to catecholamines and may exert mineralocorticoid effects at high levels.
- Clinical Picture: Central obesity, “moon face,” buffalo hump, purple striae, and easy bruising.
- Logic: Screening involves the overnight dexamethasone suppression test or 24-hour urinary free cortisol. An elevated late-night salivary cortisol is also a highly effective screening tool.
Obstructive Sleep Apnea (OSA)
OSA is an independent risk factor for hypertension and is present in a large proportion of patients with resistant hypertension. Repetitive nocturnal hypoxia leads to sympathetic activation and oxidative stress.
- Logic: Suspect in obese patients with loud snoring, morning headaches, and daytime somnolence. Screening tools like the STOP-BANG or Epworth Sleepiness Scale guide the need for definitive diagnosis via polysomnography.
Coarctation of the Aorta
This mechanical narrowing of the aorta should be excluded in any young patient with hypertension.
- Logic: The diagnostic cornerstone is the physical exam—simultaneous palpation of brachial and femoral pulses. A delay or weakening of the femoral pulse relative to the brachial pulse (radio-femoral delay) is pathognomonic.
- Imaging: Chest X-ray may show rib notching (from collateral circulation) or the “3-sign” of the aortic knuckle. Echocardiography, CT, or MRI can characterize the degree of narrowing and the pressure gradient.
Thyroid and Parathyroid Pathologies
Both hyperthyroidism and hypothyroidism can result in hypertension, though through different mechanisms. Hyperthyroidism increases cardiac output and systolic pressure, whereas hypothyroidism increases peripheral resistance and diastolic pressure.
- Hyperparathyroidism: Hypertension is common in this state, possibly due to the direct effects of hypercalcemia on vascular smooth muscle tone.
- Logic: Routine screening of TSH and serum calcium is advised when clinical suspicion (e.g., tremors, lethargy, or renal calculi) is present.
Drug-Induced and Toxicological Factors
A careful review of all ingested substances is mandatory, as many commonly used agents can raise blood pressure or interfere with therapy.
| Substance Class | Mechanism of Hypertension |
| NSAIDs | Inhibition of vasodilatory prostaglandins; sodium and water retention. |
| Oral Contraceptives | Progesterone effects on small vessels and RAAS stimulation. |
| Sympathomimetics | Decongestants (pseudoephedrine) and weight-loss drugs. |
| Illicit Drugs | Cocaine and amphetamines cause acute sympathetic surges. |
| Herbal Supplements | Licorice (pseudohyperaldosteronism), ephedra, and ginseng. |
| Alcohol | Chronic excess has a J-shaped relationship; withdrawal causes sympathetic overactivity. |
Conclusion: Synthesizing the MASTERplan for Diagnostic Precision
The diagnostic approach to arterial hypertension is a multi-dimensional task that requires the clinician to move from simple measurement to sophisticated physiological reasoning. By utilizing the ESH/ESC “MASTERplan”—Measure, Assess risk, Screen for secondary causes, Target organ damage evaluation, and Evaluate for adherence—the clinician can navigate the complexities of this condition.
The exhaustive differentiation of secondary hypertension is not a “shotgun” approach of ordering every test for every patient. Instead, it is a targeted, logical progression. It begins with the identification of “red flags” and proceeds through high-sensitivity screening tests (like the ARR for aldosteronism or metanephrines for pheochromocytoma) before moving to high-specificity confirmatory imaging. In doing so, the clinician transforms the management of hypertension from a routine exercise in blood pressure reduction into a precise medical intervention that addresses the underlying pathology, improves prognostic outcomes, and, in many cases, offers a definitive cure for the symptomatic patient.