Description
Physiological and Technical Standards in Pulmonary Function Testing: A Comprehensive Clinical Perspective
The respiratory system operates as a finely tuned biological engine, facilitating the vital exchange of gases necessary to sustain cellular life. Within the clinical environment, the assessment of this system relies heavily on the objective data provided by pulmonary function testing (PFT). These investigations serve as an indispensable bridge between physiological theory and clinical practice, allowing the physician to quantify impairment, diagnose pathology, and tailor therapeutic interventions to the specific needs of the patient. In the spirit of the ancient physicians who sought balance and understanding, modern clinicians must look beyond the mere numbers on a report to the underlying mechanisms that govern respiratory health. Pulmonary function testing is not merely a collection of measurements but a diagnostic window into the mechanical, vascular, and gas-exchanging properties of the lungs.
The following treatise provides an exhaustive analysis of the physiological basis, technical performance, and clinical interpretation of pulmonary function tests, integrated with the latest international standards and evidence-based therapeutic strategies. It is designed for medical professionals and students who seek a nuanced understanding of respiratory diagnostics within the framework of modern internal medicine.
The Physiological Foundations of Respiratory Mechanics
To appreciate the utility of pulmonary function testing, one must first comprehend the complex interrelationships among the elements that maintain homeostasis in the respiratory system. Breathing involves a coordinated effort between the brain’s respiratory centers, the motor nerves, the muscles of respiration, the thoracic cage, and the lung parenchyma itself. This integrated pump functions to move air through conducting pathways to the alveoli, where gas exchange occurs across the delicate alveolar-capillary membrane.
The mechanical properties of the lungs are determined by two primary forces: airway resistance and lung compliance. Airway resistance ($R_{aw}$) is an estimate of the friction produced between the air and the conducting pathways, while tissue resistance ($R_{tiss}$) represents the viscosity of the lung parenchyma. Clinically, $R_{aw}$ is measured using plethysmography and is found to vary inversely with lung volume. As the lungs inflate, the bronchi widen due to the increased radial traction on their outer walls, leading to a decrease in resistance. Conversely, at lower lung volumes, resistance increases. Normal values for $R_{aw}$ are typically less than 3.0 $cm~H_2O/L/sec$, and specific conductance ($SG_{aw}$) is generally greater than 0.13 $L/sec/cm~H_2O$.
Lung elasticity, or compliance, reflects the ease with which the lungs can be inflated. Inspiration is an active process requiring muscular effort to overcome the inward elastic recoil of the lungs and the outward recoil of the chest wall. Expiration is normally passive, driven by the stored elastic energy within the lung tissue. In diseases such as emphysema, where alveolar walls are destroyed, the lungs lose their elastic recoil and become “floppy,” leading to increased compliance ($C_{Lst}$). In contrast, interstitial lung diseases (ILD) lead to parenchymal stiffening, which significantly reduces compliance and makes the lungs difficult to inflate.
Classification of Respiratory Pathophysiology
From the perspective of Harrison’s Principles of Internal Medicine, most respiratory diseases can be categorized based on their physiological patterns: obstructive, restrictive, or vascular.
Obstructive Pathophysiology
Obstructive lung diseases are characterized by persistent airflow limitation, primarily during expiration. This occurs because of narrowing of the airways (as in asthma or chronic bronchitis) or a loss of the elastic support that keeps the small airways open during exhalation (as in emphysema). The physiological hallmark of obstruction is a reduction in the $FEV_1/FVC$ ratio. Air trapping is a frequent consequence, often leading to an increase in residual volume (RV) and, in severe cases, the functional residual capacity (FRC).
Restrictive Pathophysiology
Restrictive disorders are defined by a reduction in total lung capacity (TLC). These can be subdivided into intrinsic and extrinsic causes. Intrinsic restriction occurs within the lung parenchyma, where inflammation or fibrosis destroys healthy tissue, as seen in idiopathic pulmonary fibrosis (IPF). Extrinsic restriction results from factors outside the lungs that impede their expansion, such as pleural effusions, chest wall deformities like kyphoscoliosis, or neuromuscular diseases like myasthenia gravis and amyotrophic lateral sclerosis (ALS).
Vascular Pathophysiology
Abnormalities of the pulmonary vasculature, such as pulmonary hypertension or pulmonary embolism, primarily affect gas exchange and diffusing capacity rather than the mechanical volumes and flows of the lungs. These conditions often present with an isolated reduction in $DL_{CO}$ despite normal spirometry and lung volumes.
The Measurement of Lung Volumes and Capacities
Quantifying the static volumes of air contained within the lungs is essential for the definitive diagnosis of restrictive lung disease and the assessment of hyperinflation in obstructive states. While spirometry can measure the volumes that the patient can actively inhale or exhale, it cannot measure the volume of air that remains in the lungs after a maximal exhalation—the residual volume (RV).
Primary Volumes and Their Clinical Significance
| Volume/Capacity | Definition | Clinical Implication |
| Total Lung Capacity (TLC) | Total volume of gas in the lungs after a maximum inhalation. | Decreased in restriction; increased in emphysema. |
| Residual Volume (RV) | Volume of gas remaining in the lungs after a maximum exhalation. | Increased in air trapping; signifies small airway closure. |
| Functional Residual Capacity (FRC) | Volume of gas in the lungs at the end of a spontaneous expiration. | Represents the resting mechanical balance of the thorax. |
| Vital Capacity (VC) | The maximum amount of air that can be inhaled or exhaled. | Non-specific marker; decreased in both obstruction and restriction. |
TLC is determined by the balance between the strength of the inspiratory muscles and the elastic recoil of the respiratory system. FRC corresponds to the point where the inward recoil of the lungs is exactly counterbalanced by the outward recoil of the chest wall. RV is limited by the ability of the expiratory muscles to compress the chest wall and the tendency of the airways to collapse at low volumes.
Technical Assessment of FRC
The functional residual capacity serves as the starting point for calculating TLC and RV. It is measured in the pulmonary function laboratory using one of three techniques:
- Body Plethysmography: The patient sits in an airtight cabin and performs gentle panting maneuvers against a closed shutter. By measuring the changes in pressure at the mouth and inside the cabin, the total volume of compressible gas in the thorax is calculated using Boyle’s Law ($P_1V_1 = P_2V_2$). This method is the “gold standard” because it includes air that is trapped behind closed or non-communicating airways.
- Helium Dilution: The patient breathes from a closed circuit containing a known concentration of helium. As the helium equilibrates with the air in the lungs, its concentration drops proportionally to the lung volume. This method only measures ventilated lung volume and may underestimate FRC in patients with severe obstruction.
- Nitrogen Washout: The patient breathes 100% oxygen, which gradually replaces the nitrogen resident in the lungs. The exhaled gas is collected, and the total volume of nitrogen washed out is used to calculate the starting lung volume. Like helium dilution, this may underestimate volumes in the presence of significant air trapping.
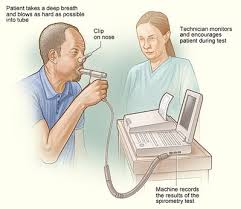
Spirometry: Technical Execution and Quality Standards
Spirometry remains the most common PFT due to its ability to provide immediate, reliable information regarding overall mechanical function. However, it is an effort-dependent test that requires skilled coaching and patient motivation to ensure clinical validity.
Procedural Steps and Acceptability Criteria
A standard spirometry session involves a maximal inhalation followed by a forceful, rapid exhalation into the device. According to the 2022 ATS/ERS updates, several criteria must be met for a maneuver to be considered acceptable :
- Good Start: The exhalation must be explosive, with an extrapolated volume (the volume lost before peak flow) of less than 5% of the FVC or 150 mL (whichever is greater).
- Maximal Effort: The patient must provide maximal expiratory effort throughout the entire maneuver.
- End-of-Test Criteria: The exhalation must continue until the volume-time curve shows a plateau (no change in volume $> 0.025~L$ for at least 1 second) and the patient has exhaled for at least 6 seconds (or 3 seconds for children under 10).
- Absence of Artifacts: The maneuver must be free from coughing in the first second, glottis closure, or premature termination.
Repeatability Standards
To ensure that the results reflect the patient’s true physiological state rather than variability in effort, at least three acceptable maneuvers must be performed. The difference between the two highest $FEV_1$ values and the two highest FVC values must be within 150 mL (or 100 mL if the FVC is less than 1.0 L).
Maximal Expiratory Flow-Volume (MEFV) Curve Analysis
The MEFV curve plots instantaneous airflow against lung volume, providing a visual representation of the mechanical limitations of the respiratory system. The curve is divided into two distinct portions:
- Effort-Dependent Portion: The early part of exhalation (from TLC to about 75% of VC). The flow rate here is determined by the high elastic recoil of the inflated lung and the strength of the expiratory muscles.
- Effort-Independent Portion: The remainder of the exhalation (below 75% of VC). Once the lungs have emptied about 25%, a dynamically regulated orifice size is reached, and airflow reaches a maximum plateau regardless of further muscular effort. This is caused by dynamic airway compression at the “equal pressure point,” where the pressure surrounding the airways equals the pressure within them.
In chronic obstructive pulmonary diseases, the MEFV curve typically becomes “concave” to the volume axis, reflecting a rapid decrease in flow as lung volumes diminish. In restrictive diseases, the curve appears narrowed but maintains a high flow rate relative to the reduced volume.
The Modern Interpretive Paradigm: Z-Scores and Race-Neutrality
The interpretation of PFTs has undergone a fundamental shift in recent years, moving away from fixed percentage thresholds toward more mathematically rigorous and biologically appropriate benchmarks.
From Fixed Percentages to Z-Scores
Historically, a value $> 80\%$ of predicted was considered “normal.” This approach, however, fails to account for the fact that the variance of lung function measurements in a healthy population increases with age. For instance, a 70% predicted $FEV_1$ might be entirely normal for an 80-year-old but highly pathological for a 20-year-old.
The 2022 ATS/ERS technical standards advocate for the use of Z-scores, which express a measurement’s deviation from the mean in terms of standard deviation units. A Z-score of $-1.645$ corresponds to the 5th percentile of the healthy population and is defined as the Lower Limit of Normal (LLN).
Standardized Severity Grading
The updated severity grading system for all PFT parameters (including $FEV_1$, FVC, and $DL_{CO}$) is based on Z-score thresholds rather than fixed percent-predicted slabs.
| Severity Descriptor | Z-Score Range | Clinical Context |
| Normal | $\geq -1.645$ | Within the 5th percentile of healthy non-smokers. |
| Mild | $-1.65$ to $-2.5$ | Slight impairment; often asymptomatic at rest. |
| Moderate | $-2.51$ to $-4.0$ | Clinically significant; likely to manifest with exertional dyspnea. |
| Severe | $< -4.0$ | Pronounced physiological limitation; significant disability. |
The Global Lung Function Initiative (GLI) and Race-Neutrality
Perhaps the most significant ethical and clinical evolution in the field is the transition to race-neutral reference equations. For decades, PFT software used race-specific adjustments, typically assuming that Black and Asian individuals had lower lung function purely due to ancestry. Recent research suggests that these differences are often rooted in social determinants of health, environmental exposures, and socioeconomic status rather than innate biology.
The ATS now recommends the use of the “GLI Global” (2022) weighted race-composite average equation. Switching to this race-neutral approach has profound implications for equity. For example, Black and Southeast Asian individuals are more likely to be diagnosed with impairment under GLI Global, as they are no longer being compared to a lower, race-adjusted “normal”. This shift ensures that more patients receive appropriate care, disability recognition, and access to therapeutic trials.
Diffusing Capacity of the Lung for Carbon Monoxide ($DL_{CO}$)
The $DL_{CO}$ test measures the efficiency with which gases transfer from the alveolar air into the pulmonary capillary blood. It assesses the integrated function of the alveolar surface area, the thickness of the blood-gas barrier, and the volume of blood in the pulmonary capillaries.
Physiological Components of $DL_{CO}$
The $DL_{CO}$ measurement reflects two processes occurring in series:
- Membrane Conductance ($D_M$): Represents the molecular diffusion of gas across the alveolar epithelium, interstitium, and capillary endothelium. This component depends primarily on the total surface area available for exchange and the thickness of the barrier.
- Reactive Conductance ($\theta \times V_c$): Represents the chemical combination of carbon monoxide with hemoglobin within the red blood cells. This component is functionally an indicator of pulmonary capillary blood flow.
Normally, about 75-80% of the resistance to diffusion lies in the reactive (perfusion) component, meaning $DL_{CO}$ is highly sensitive to changes in pulmonary blood volume.
Clinical Interpretation of $DL_{CO}$ Abnormalities
A low $DL_{CO}$ is a highly sensitive but non-specific indicator of parenchymal or vascular disease. To clarify the diagnosis, clinicians often look at $K_{CO}$ (the transfer coefficient, $DL_{CO}/V_A$) and $V_A$ (alveolar volume).
- Emphysema: Low $DL_{CO}$ and low $K_{CO}$ despite hyperinflation. This results from the destruction of alveolar walls and loss of surface area.
- Interstitial Lung Disease: Low $DL_{CO}$ due to both reduced lung volume ($V_A$) and increased thickness of the diffusion barrier. $K_{CO}$ is typically reduced.
- Pulmonary Vascular Disease: Low $DL_{CO}$ and low $K_{CO}$ with normal spirometry and lung volumes. This is a hallmark of pulmonary hypertension or chronic thromboembolic disease.
- Neuromuscular Disease: Low $DL_{CO}$ but high or normal $K_{CO}$. Because the lung parenchyma is healthy but cannot expand fully, the blood flow per unit of ventilated lung volume is actually increased.
$DL_{CO}$ is also affected by acute clinical factors. It decreases with anemia (fewer binding sites) and increases with polycythemia or alveolar hemorrhage (more binding sites). It must be corrected for hemoglobin levels and the presence of carboxyhemoglobin (from smoking) to avoid spuriously low results.
Gas Exchange and Arterial Blood Gases
The ultimate purpose of the respiratory system is to preserve functional homeostasis by maintaining constant blood gas tensions. Direct assessments of gas exchange involve measuring the partial pressures of oxygen ($P_aO_2$) and carbon dioxide ($P_aCO_2$) in arterial blood.
The Alveolar-Arterial Oxygen Gradient ($A-aDO_2$)
The $A-aDO_2$ is a critical calculation that differentiates between causes of hypoxemia. It is computed as the difference between the calculated alveolar oxygen tension ($P_AO_2$) and the measured arterial oxygen tension ($P_aO_2$).
$$P_AO_2 = P_IO_2 – \left$$
Normal values for $A-aDO_2$ are typically less than 30 mmHg but increase linearly with age, ranging from 6-10 mmHg in a 20-year-old to 26-30 mmHg in a 70-year-old.
Causes of Hypoxemia
| Cause | PaCO2 | A−aDO2 | Response to 100% O2 |
| Low Inspired $O_2$ (High Altitude) | Normal/Low | Normal | Excellent |
| Hypoventilation (CNS/Neuromuscular) | High | Normal | Excellent |
| Diffusion Limitation (Severe ILD) | Normal/Low | Elevated | Good |
| $V/Q$ Mismatch (COPD/Pneumonia) | Variable | Elevated | Excellent |
| Right-to-Left Shunt (Cardiac/Pulmonary) | Normal/Low | Elevated | Poor |
In cases of central alveolar hypoventilation (e.g., opioid overdose or neuromuscular weakness), the decrease in $P_aO_2$ is proportional to the increase in $P_aCO_2$, keeping the $A-aDO_2$ within the normal range. An elevated $A-aDO_2$ always signifies intrinsic lung or vascular pathology.
Respiratory Muscle Function and Strength
Many patients present with restrictive patterns on PFTs not because of lung disease, but because of a failure of the ventilatory pump. Respiratory muscle weakness can be assessed through the measurement of maximal static pressures.
- Maximal Inspiratory Pressure ($P_{Imax}$ or MIP): Measured during a maximal inspiratory effort against a closed system at RV. It reflects the strength of the diaphragm and accessory inspiratory muscles.
- Maximal Expiratory Pressure ($P_{Emax}$ or MEP): Measured during a maximal expiratory effort at TLC. It reflects the strength of the abdominal and intercostal muscles.
Normal values for MIP are generally less than $-70~cm~H_2O$ in young men and $-35~cm~H_2O$ in young women. MEP should be greater than $90~cm~H_2O$ in men and $50~cm~H_2O$ in women. A significant decline in vital capacity when moving from an upright to a supine position (often $> 20\%$) is a specific clinical sign of diaphragmatic weakness or paralysis.
Exercise Performance Testing: Surrogates and CPET
Exercise testing is employed to evaluate the integrated performance of the heart, lungs, and skeletal muscles, particularly in patients with unexplained dyspnea.
The 6-Minute Walk Test (6-MWT)
The 6-MWT measures the maximal distance a person can walk in six minutes at their own pace. While simple and reflecting activities of daily living, it does not provide specific information regarding the etiology of limitation. It is primarily used to monitor response to rehabilitation and to establish oxygen requirements during exertion.
Cardiopulmonary Exercise Testing (CPET)
CPET provides a comprehensive physiological profile during graded work on a treadmill or cycle ergometer. Key measurements include:
- Peak $VO_2$: The maximal rate of oxygen consumption. It is the gold standard for assessing aerobic capacity.
- Anaerobic Threshold (AT): The point at which metabolism shifts from aerobic to anaerobic, signifying the onset of metabolic acidosis. A low AT (often $< 40\%$ of predicted $VO_2$) suggests poor $O_2$ delivery to the tissues.
- Ventilatory Equivalent for $CO_2$ ($V_E/VCO_2$): A marker of efficient ventilation. High values reflect wasted ventilation (increased dead space) or hyperventilation.
- Oxygen Pulse: The ratio of $VO_2$ to heart rate, which acts as a surrogate for stroke volume.
Patterns of CPET results allow the clinician to distinguish between deconditioning, cardiac failure, and primary lung disease. For instance, patients with COPD are typically limited by a lack of ventilatory reserve, while cardiac patients reach their maximal predicted heart rate before exhausting their ventilation.
Bronchial Provocation and Airway Reactivity
For patients with normal spirometry but clinical symptoms suggestive of asthma, bronchial provocation testing is used to demonstrate hyperresponsiveness.
Methacholine Challenge
Methacholine, a muscarinic agonist, is administered in increasing concentrations. The primary outcome is the $PC_{20}$—the provocative concentration required to cause a 20% drop in $FEV_1$. A $PC_{20}$ of $\leq 16~mg/mL$ is generally considered abnormal. A negative methacholine challenge during a period when the patient is symptomatic virtually rules out the diagnosis of asthma.
Differential Diagnosis: The French’s Index Framework
Constructing a differential diagnosis requires a systematic ranking of probabilities based on the patient’s primary symptom, age, and risk factors. Using the analytical methodology of French’s Index, we categorize the causes of dyspnea and chronic cough to guide the diagnostic workup.
Differential Diagnosis of Dyspnea
| Etiology | Frequency/Probability | Key Diagnostic Clues |
| Asthma/COPD | Very High | Wheezing, tobacco use, reversibility on spirometry. |
| Congestive Heart Failure | High | Orthopnea, rales, elevated BNP, peripheral edema. |
| Pneumonia | Moderate | Fever, productive cough, lung consolidations on CXR. |
| Pulmonary Embolism | Moderate/Critical | Sudden onset, pleuritic pain, elevated D-dimer. |
| Interstitial Lung Disease | Low/Moderate | Progressive exertional dyspnea, dry cough, Velcro crackles. |
| Anxiety/Hyperventilation | Moderate | Sighing respirations, normal ABG and PFTs. |
The temporal course of dyspnea is crucial. Acute onset suggests laryngeal edema, pneumothorax, or pulmonary embolism. Gradual progression over years is the hallmark of COPD or fibrotic lung disease.
Differential Diagnosis of Chronic Cough
Chronic cough (defined as $> 8$ weeks) is often a diagnostic challenge. The “Big Three” causes account for the majority of cases.
- Upper Airway Cough Syndrome (UACS): Previously known as postnasal drip. Clues include frequent throat clearing and a cobblestone nasopharynx. It should be treated first empirically with antihistamines or nasal steroids.
- Asthma (Cough-Variant): Cough is the sole manifestation. Diagnosis often requires methacholine challenge or a trial of inhaled corticosteroids.
- Gastroesophageal Reflux Disease (GERD): Often “silent” (no heartburn). Cough is triggered by meals, talking, or lying down. A 2-week trial of high-dose proton pump inhibitors (PPI) is often diagnostic.
In smokers, the possibility of bronchogenic carcinoma must always be considered if the character of a chronic cough changes, regardless of other findings.
Physical Examination and Physical Diagnostics
While PFTs provide objective data, the physical examination provides the context. In the realm of pulmonary diagnostics, certain findings are quintessential.
- Auscultation: Bibasilar “Velcro” crackles are the early hallmark of IPF. Wheezing indicates turbulent flow through narrowed airways, while diminished breath sounds suggest emphysema or a large pleural effusion.
- Tactile Fremitus: Increased fremitus suggests consolidation (e.g., pneumonia), while decreased fremitus suggests a barrier between the lung and the chest wall (e.g., pleural effusion or pneumothorax).
- Chest Wall Dynamics: The use of accessory muscles (sternocleidomastoids and scalenes) and supraclavicular retractions are markers of severely increased work of breathing, common in exacerbations of asthma or COPD.
- Clubbing: The bulbous enlargement of the fingertips is a sign of chronic hypoxia and is frequently associated with bronchiectasis, lung cancer, and idiopathic pulmonary fibrosis.
Laboratory and Instrumental Correlation
A comprehensive diagnosis integrates PFTs with laboratory and imaging findings.
- Imaging: High-Resolution Computed Tomography (HRCT) is the gold standard for diagnosing parenchymal lung disease. A “Usual Interstitial Pneumonia” (UIP) pattern, characterized by subpleural, basal-predominant reticular abnormalities and honeycombing, is required for the diagnosis of IPF. In COPD, CT can quantify the extent of emphysematous destruction.
- Laboratory Data:
- Brain Natriuretic Peptide (BNP): Highly useful for excluding heart failure in the dyspneic patient.
- Blood Eosinophil Count (BEC): A critical marker for therapeutic selection in COPD; patients with BEC $\geq 300~cells/\mu L$ show better responses to inhaled corticosteroids.
- D-Dimer: Used to rule out pulmonary embolism in patients with low-to-intermediate pre-test probability.
Evidence-Based Therapeutic Strategies
Once the physiological impairment has been quantified and the diagnosis established, management is guided by current international protocols.
Asthma Management (GINA 2024 Updates)
The most significant recent change in asthma therapy is the strong recommendation against the use of SABA as monotherapy. Regular use of SABAs leads to beta-receptor downregulation and increased risk of severe exacerbations.
Track 1 (Preferred Strategy): The use of low-dose Inhaled Corticosteroid (ICS)-Formoterol as both maintenance and reliever therapy (MART/SMART). This ensures that every time a patient uses their “rescue” inhaler, they also receive an anti-inflammatory dose.
Track 2 (Alternative Strategy): The use of SABA as the reliever, provided it is always accompanied by a separate daily maintenance ICS.
| Severity Step | Preferred Treatment (Track 1) | Alternative Treatment (Track 2) |
| Steps 1-2 | As-needed low-dose ICS-Formoterol. | Daily low-dose ICS plus as-needed SABA. |
| Step 3 | Maintenance + reliever low-dose ICS-Formoterol. | Maintenance ICS-LABA plus as-needed SABA. |
| Step 4 | Maintenance + reliever medium-dose ICS-Formoterol. | Maintenance medium-dose ICS-LABA + as-needed SABA. |
| Step 5 | Add LAMA; consider biologic therapies (e.g., Omalizumab, Dupilumab). | Add LAMA; consider biologics. |
COPD Management (GOLD 2025 Updates)
Stable COPD management is now focused on symptom reduction and exacerbation prevention, with an emphasis on early dual bronchodilation.
- Group A (Low Symptoms/Low Risk): A single bronchodilator (SABA or SAMA as needed).
- Group B (High Symptoms/Low Risk): Dual bronchodilation with LAMA + LABA is now the standard.
- Group E (High Risk/Regardless of Symptoms): LAMA + LABA is the preferred initial therapy. ICS should be added only if the BEC is $\geq 300~cells/\mu L$.
Triple therapy (ICS/LAMA/LABA) has been shown to reduce mortality and exacerbation rates in patients with frequent events and high BEC. Novel biological therapies, such as Dupilumab, are now proposed for patients with a chronic bronchitis phenotype and BEC $\geq 300~cells/\mu L$ who remain symptomatic on triple therapy.
Interstitial Lung Disease and IPF Management
In contrast to obstructive diseases, ILD management focuses on slowing the progression of fibrosis.
| Drug | Recommended Dosage | Clinical Rationale |
| Nintedanib | 150 mg twice daily (BID) with food. | Tyrosine kinase inhibitor; slows the annual decline of FVC. |
| Pirfenidone | Titrated to 801 mg three times daily (TID) with food. | Reduces fibroblast proliferation and collagen synthesis. |
Common side effects of Nintedanib include significant diarrhea (occurring in about two-thirds of patients) and liver enzyme elevation. Pirfenidone is primarily associated with photosensitivity and gastrointestinal upset.
Safety and Pharmacological Vigilance
The management of complex respiratory patients often involves multiple medications, creating a high risk for clinically significant drug-drug interactions (DDIs).
Significant Respiratory Drug Interactions
- Theophylline and Beta-Blockers: This is one of the most dangerous interactions in pulmonology. Non-selective beta-blockers (e.g., Propranolol) can reduce theophylline clearance by up to 50%, leading to seizures, arrhythmias, and nausea. Furthermore, they antagonize the bronchodilatory effects of theophylline and beta-agonists.
- Beta-Blockers in Asthma vs. COPD: While any history of asthma is considered a contraindication to beta-blocker use (due to the risk of fatal bronchospasm), cardio-selective agents (e.g., Bisoprolol or Metoprolol) are safe and recommended for patients with COPD and heart failure.
- Theophylline and Antibiotics: The clearance of theophylline is inhibited by certain macrolides (e.g., Erythromycin) and cimetidine, which can rapidly lead to toxic serum levels.
- Steroids and Hypokalemia: The concurrent use of systemic corticosteroids and high-dose beta-agonists (like Salbutamol) can lead to severe hypokalemia, as both classes promote the intracellular shift of potassium.
Conclusion
The clinical utility of pulmonary function testing extends far beyond the diagnostic identification of obstruction and restriction. It provides a foundational understanding of a patient’s unique physiological limitations, allowing for precision in the application of modern therapeutic guidelines. As we have transitioned into the era of Z-scores and race-neutral reference equations, our ability to identify impairment across diverse populations has reached unprecedented accuracy.
For the clinician, the PFT report is not the end of the diagnostic journey but a call to integrate clinical signs, risk factors, and imaging into a cohesive understanding of the patient’s condition. As chronic respiratory diseases continue to rise in prevalence globally, the mastery of these functional assessments remains essential to the ethical and effective practice of internal medicine. The overarching goal remains the restoration of physiological balance and the preservation of the patient’s quality of life through informed, evidence-based care.