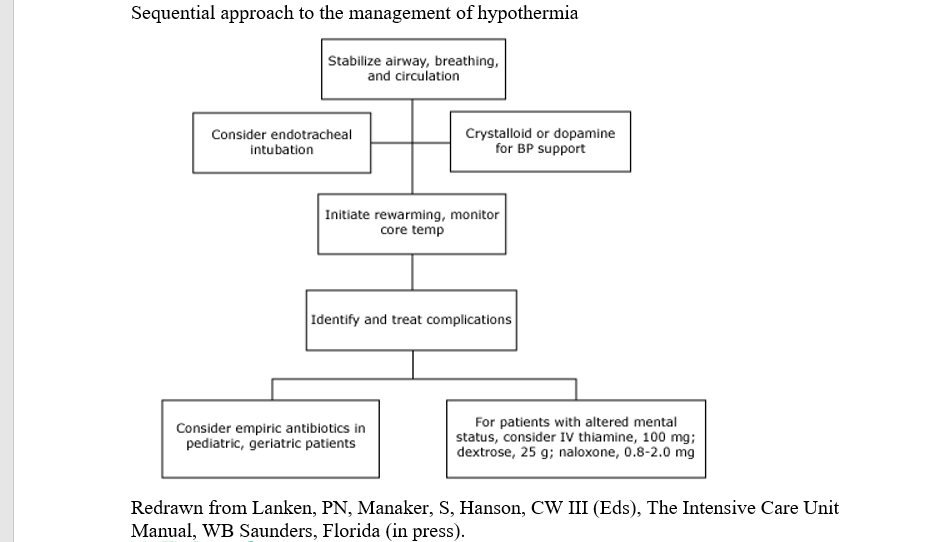
Description
Clinical Pathophysiology and Integrated Management of Accidental Hypothermia: An Expert Review for Medical Practitioners
The maintenance of a constant internal thermal environment is among the most sophisticated evolutionary achievements of the human organism. This homeostatic resilience, centered within the hypothalamus, allows for the precise execution of biochemical reactions that sustain life. When this equilibrium is disrupted by environmental exposure or underlying metabolic failure, the resulting syndrome of accidental hypothermia—defined as a core body temperature falling below $35^{\circ}C$ ($95^{\circ}F$)—initiates a complex cascade of physiological deterioration. For the clinician, managing such patients requires more than just rewarming; it demands a deep understanding of thermodynamics, cellular metabolic suppression, and the delicate interplay between conventional pharmacology and the body’s innate adaptive recovery mechanisms. Guided by the principle of “Primum non nocere,” this report synthesizes the golden standards of internal medicine with an empathetic, holistic approach to patient care.
The Thermodynamic Balance: Heat Production and Dissipation
Human life exists within a narrow thermal window where heat production must precisely match heat loss. This balance is not merely a matter of comfort but a requirement for the structural integrity of proteins and the kinetics of enzymatic reactions. According to the principles established in Harrison’s Principles of Internal Medicine, heat is primarily generated by cellular metabolism, with the heart and liver being the most prolific contributors during rest. During cold stress, the body attempts to increase this production through mechanical work—shivering—which can elevate the metabolic rate by up to 500%.
The dissipation of heat occurs through four physical mechanisms, each dictated by the laws of physics and environmental conditions. Radiation involves the emission of infrared energy and accounts for 65% of heat loss in a neutral, dry environment. Conduction, the direct transfer of heat to an adjacent cooler object, is the primary driver of cooling in immersion scenarios; water conducts heat approximately 25 times faster than air, leading to a rapid decline in core temperature. Convection refers to the loss of heat to moving air or water currents, which continually replace the warmed layer of air surrounding the body with cooler molecules. Finally, evaporation through the skin and respiratory tract accounts for significant loss, particularly when humidity is low or during high-exertion states.
| Mechanism | Description | Clinical Context in Hypothermia |
| Radiation | Emission of electromagnetic infrared energy. | Primary loss mechanism in dry, still air; influenced by skin exposure. |
| Conduction | Direct heat transfer between contacting surfaces. | Critically accelerated in water immersion or contact with cold ground. |
| Convection | Heat transfer via moving air or fluid currents. | “Wind chill” effect; movement in water accelerates core cooling. |
| Evaporation | Cooling via vaporization of moisture. | Important in cold, dry climates and in patients with skin barrier defects (burns). |
The metabolic response to this cooling is characterized by the $Q_{10}$ effect. For every $10^{\circ}C$ drop in core temperature, the metabolic rate of the brain and whole body decreases by a factor of approximately 2 to 2.2. While this reduction in $O_{2}$ consumption ($V_{O_{2}}$) and $CO_{2}$ production ($V_{CO_{2}}$) provides a degree of neuroprotection during periods of low flow, it also complicates the management of acid-base balance and the administration of medications.
Pathophysiology of Multisystemic Failure
As the core temperature descends, every organ system undergoes predictable yet profound alterations. Understanding “why” and “how” these changes occur is essential for the clinician to anticipate complications rather than merely reacting to them.
Cardiovascular Dynamics and Myocardial Irritability
The initial response to cold is a sympathetic surge, leading to tachycardia and peripheral vasoconstriction. This is the body’s attempt to preserve core heat by sacrificing the periphery. However, as cooling continues into the moderate and severe stages, the pacemaker cells in the sinoatrial node demonstrate a decrease in spontaneous depolarization, leading to a progressive, temperature-dependent bradycardia. This bradycardia is notably refractory to atropine, as the mechanism is not vagally mediated but is a result of direct metabolic suppression.
The hypothermic myocardium becomes exquisitely sensitive to mechanical stimulation. Rough handling, tracheal intubation, or the placement of central venous catheters can precipitate ventricular fibrillation (VF). This irritability is linked to the prolongation of the action potential and the development of significant transmural voltage gradients, which manifest on the electrocardiogram (ECG) as the Osborn J wave. Furthermore, as the temperature drops below $30^{\circ}C$, the heart becomes less responsive to defibrillation and vasopressors, necessitating a focus on rewarming as the primary antiarrhythmic therapy.
Respiratory and Acid-Base Shifts
Initially, cold exposure triggers tachypnea and hyperventilation, but as the core temperature falls, the respiratory rate and tidal volume decline. The protective cough and gag reflexes are progressively lost, increasing the risk of aspiration pneumonia. A significant challenge in management is the “alpha-stat” vs. “pH-stat” approach to blood gas analysis. Because gas solubility increases as temperature decreases, a cold patient will have a higher pH and a lower $P_{O_{2}}$ and $P_{CO_{2}}$ than measured by a laboratory analyzer warmed to $37^{\circ}C$. For adult patients, the consensus remains to use uncorrected values (measured at $37^{\circ}C$) to guide clinical decisions, as these values reflect the electrochemical neutrality of the blood.
Renal Function and “Cold Diuresis”
One of the most frequent findings in early hypothermia is an increase in urine output despite a likely state of dehydration. This “cold diuresis” occurs because peripheral vasoconstriction leads to a relative increase in central blood volume, which is sensed by the body as hypervolemia. This leads to the suppression of antidiuretic hormone (ADH) and an increase in atrial natriuretic peptide (ANP), coupled with a temperature-induced defect in the renal tubular reabsorption of water and sodium. Consequently, many hypothermic patients present with significant volume depletion and may require aggressive, warmed crystalloid resuscitation during rewarming.
Neurological Depression
The central nervous system is highly sensitive to cooling. Cerebral blood flow decreases by approximately 6-7% for every $1^{\circ}C$ drop in temperature. Clinically, this manifests as a progressive decline in the level of consciousness, from the initial confusion and ataxia of mild hypothermia to the profound coma and areflexia seen in severe cases. It is vital to remember that a patient’s neurological exam may appear consistent with brain death while they are severely hypothermic; therefore, no patient should be pronounced dead until they have been rewarmed to at least $32^{\circ}C$ to $35^{\circ}C$ and still show no signs of life.
Differential Diagnosis: Applying French’s Index
In the clinical setting, hypothermia is often the presenting symptom of a more complex underlying pathology. Using the analytical approach of French’s Index, we must distinguish between primary environmental exposure and secondary hypothermia caused by metabolic or regulatory failure. This differentiation is critical because secondary hypothermia carries a significantly higher mortality rate if the precipitating cause is not addressed.
Classification by Probability and Severity
| Category | Differential Diagnoses | Rationale and Clinical Clues |
| Most Likely | Accidental Environmental Exposure | History of cold, wet, or windy environment; presence of shivering. |
| Most Likely | Ethanol Intoxication | Vasodilation, impaired judgment, and suppressed shivering response. |
| Do Not Miss | Sepsis | Especially in the elderly; hypothermia may be the only sign of infection. |
| Do Not Miss | Hypoglycemia | Neuroglycopenia disrupts hypothalamic thermoregulation; check fingerstick glucose immediately. |
| Do Not Miss | Wernicke’s Encephalopathy | Thiamine deficiency; often associated with ethanol use and ataxia. |
| Severe/Endocrine | Myxedema Coma | Severe hypothyroidism; look for surgical scars, goiter, or history of medication. |
| Severe/Endocrine | Adrenal Insufficiency | Failure to rewarm despite aggressive measures; requires steroid replacement. |
| Rare/Neurological | Hypothalamic Injury | Stroke, trauma, or tumor affecting the thermoregulatory center. |
| Rare/Neurological | Spinal Cord Transection | Loss of autonomic control and inability to shiver below the level of injury. |
Clinical Stages and the Swiss Staging System
While core temperature measurement is the diagnostic gold standard, clinicians in the field often lack specialized equipment. The Swiss Staging System allows for the categorization of hypothermia based on clinical signs, providing a reliable proxy for temperature and guiding the risk assessment for cardiac arrest.
| Stage | Clinical Signs | Approx. Temperature | Risk of Cardiac Arrest |
| HT I (Mild) | Conscious, shivering vigorously. | $32-35^{\circ}C$ | Low. |
| HT II (Moderate) | Impaired consciousness, no shivering. | $28-32^{\circ}C$ | Moderate. |
| HT III (Severe) | Unconscious, vital signs present. | $24-28^{\circ}C$ | High. |
| HT IV (Severe) | No detectable vital signs (apparent death). | $<24^{\circ}C$ | Arrest present. |
The presence of shivering is a vital diagnostic clue; if a patient is shivering, their core temperature is almost certainly above $30^{\circ}C$, and their metabolic engine is still attempting to generate heat. Conversely, the loss of shivering in a cold patient is an ominous sign of metabolic exhaustion or progression into the moderate stage of hypothermia.
Diagnostic Evaluation and the Electrocardiographic Signature
Accurate diagnosis requires a low-reading thermometer, as standard clinical thermometers often stop at $34^{\circ}C$. For patients with a secured airway, esophageal probes are preferred for their proximity to the heart, though their placement must be distal to the level of the trachea to avoid cooling from ventilation.
The Osborn Wave
The most distinctive ECG finding in hypothermia is the Osborn J wave. This deflection occurs at the R-ST junction and is most prominent in leads $V_{2}-V_{5}$ and the inferior leads. While its presence is highly suggestive of hypothermia, its amplitude is inversely proportional to the core temperature. Pathophysiologically, the J wave represents a transmural voltage gradient during early repolarization, caused by the heterogeneous distribution of the transient outward potassium current ($I_{to}$) across the ventricular wall. It is essential to recognize that computer-interpreted ECGs often mistake Osborn waves for ST-segment elevation indicative of myocardial infarction.
Laboratory Findings and the “37°C Trap”
Laboratory values in hypothermia must be interpreted with caution. Hemoconcentration is common, leading to a deceptively high hematocrit. However, the most critical “trap” involves coagulation studies. Coagulation enzymes are temperature-dependent, and while a patient may be bleeding uncontrollably in the operating room (at $30^{\circ}C$), their PT and PTT results will come back from the lab as “normal” because the test was performed in a $37^{\circ}C$ incubator. Clinicians should assume a functional coagulopathy is present and focus on rewarming rather than just the administration of clotting factors.
| Lab Parameter | Finding in Hypothermia | Clinical Implication |
| Glucose | Variable (Hyper/Hypo) | Shivering consumes glucose; hypothermia inhibits insulin. |
| Potassium | Often Elevated | Hyperkalemia $>12$ mmol/L in arrest is a marker of futility. |
| Amylase/Lipase | Often Elevated | Reflects hypothermia-induced pancreatitis or microvascular ischemia. |
| Hematocrit | Elevated | Due to plasma shift and cold diuresis; masks anemia. |
| WBC/Platelets | Decreased | Splenic and hepatic sequestration; not bone marrow failure. |
Comprehensive Management: The Rewarming Hierarchy
The management of hypothermia is a tiered process, moving from non-invasive to invasive techniques based on the severity of the thermal deficit and the stability of the patient.
Passive External Rewarming (PER)
This is the treatment of choice for mild hypothermia. By removing wet clothes and providing insulation with blankets, we allow the patient to use their own metabolic heat to recover. PER is only effective in patients who can still shiver and have adequate energy stores.
Active External Rewarming (AER)
Indicated for moderate hypothermia or mild hypothermia with comorbidities. This involves the application of external heat sources like forced-air blankets (Bair Huggers), radiant heat, or warm packs. A critical caution is to rewarm the trunk before the extremities to minimize “afterdrop”—the phenomenon where cold, acidotic blood from the periphery returns to the core, causing a paradoxical drop in core temperature and potential “rewarming shock”.
Active Internal Rewarming (AIR)
For severe hypothermia ($<28^{\circ}C$), AIR is necessary. This includes the administration of warmed humidified oxygen ($45^{\circ}C$) and heated intravenous fluids ($40-42^{\circ}C$). More invasive methods include peritoneal or pleural lavage with warmed saline. Left-sided pleural lavage is particularly effective as it transfers heat directly to the heart, reducing myocardial irritability.
Extracorporeal Life Support (ECLS)
In cases of hypothermic cardiac arrest or refractory instability, Cardiopulmonary Bypass (CPB) or Extracorporeal Membrane Oxygenation (ECMO) are the definitive therapies. ECLS provides not only the most rapid rewarming ($7-10^{\circ}C/hr$) but also total circulatory support, allowing the heart time to recover from the metabolic and electrolyte derangements of the cold.
Advanced Cardiac Life Support in the Cold
Resuscitating a hypothermic patient is a departure from standard ACLS. The heart is less responsive to medications, and drug metabolism is significantly slowed, leading to the risk of toxicity upon rewarming.
- Defibrillation: A single attempt at defibrillation is reasonable for VF/VT, but if unsuccessful, further attempts should be deferred until the core temperature rises above $30^{\circ}C$.
- Medications: Epinephrine and other vasopressors should be withheld or administered with doubled intervals (e.g., every 6-10 minutes) when the temperature is below $30^{\circ}C$. Once the patient is above $35^{\circ}C$, standard ACLS protocols should be followed.
- Mechanical CPR: Given the need for prolonged resuscitation (sometimes hours) during rewarming, mechanical chest compression devices are strongly recommended to ensure consistent quality and reduce rescuer fatigue.
The Holistic Perspective: Integrative Support and Herbal Safety
As the patient moves from the acute resuscitation phase to the recovery phase, we must address the profound metabolic and endocrine stress the body has endured. An integrative approach, combining traditional pharmacology with knowledge of botanical adaptogens, can facilitate the restoration of homeostasis. However, the clinician must be hyper-aware of interactions.
The Role of Adaptogens in Post-Exposure Recovery
Adaptogens are substances that help the body manage stress and return to a state of balance. During the recovery from hypothermia, the HPA axis and the thyroid gland are often significantly stressed.
- Ashwagandha (Withania somnifera): This herb is renowned for its ability to lower cortisol and support the adrenal-endocrine system. It may be particularly useful in the post-hypothermic period to manage the “catecholamine storm” that often follows rewarming.
- Rhodiola Rosea: Rhodiola helps improve physical and mental endurance by supporting ATP production and mitochondrial health. It is beneficial for patients experiencing profound fatigue after cold-induced metabolic exhaustion.
- Ginseng (Panax ginseng): Traditionally used to boost energy and immune function, ginseng can aid in the recovery of thermal regulation.
Critical Interaction Warnings and Safety
The use of herbs in the setting of critical illness requires extreme caution, particularly regarding bleeding risks and cardiovascular effects.
| Botanical Agent | Potential Interaction / Risk | Clinical Precaution |
| Ginseng | Increases bleeding risk; interacts with warfarin/aspirin. | Avoid in patients with coagulopathy or those on antiplatelet therapy. |
| Ashwagandha | May increase thyroid hormone levels; GABAergic activity. | Use caution in patients with hyperthyroidism or those taking sedatives. |
| Rhodiola | Inhibits CYP2D6 and CYP3A4 enzymes. | Can increase concentrations of co-administered psychotropic or cardiac drugs. |
| Ginkgo Biloba | Significant antiplatelet effects; interacts with many meds. | High risk of bleeding complications in the post-resuscitative phase. |
Clinicians should remind patients and students that while these natural aids offer support, they are not substitutes for physical examination and conventional treatment. Furthermore, no herbs or supplements should be given to a patient while they are still acutely hypothermic.
Complications and Prognostication
The road to recovery after severe hypothermia is fraught with potential complications. “Rewarming shock” can occur as peripheral vasodilation leads to a relative hypovolemia and acute myocardial failure. Pancreatitis and ileus are common due to microvascular ischemia and enzyme dysfunction. Disseminated Intravascular Coagulation (DIC) may also be triggered by the release of tissue factors from ischemic or brain-dead tissue.
Prognostication in the setting of cardiac arrest relies on the HOPE and ICE scores. The HOPE score, which includes age, sex, potassium, and duration of CPR, is a validated tool for determining the probability of survival after ECLS rewarming. A potassium level above $12$ mmol/L remains the most reliable indicator of irreversible cellular death and is often used to guide the ethical decision to terminate resuscitation.
Conclusion: The Path of Balance
Accidental hypothermia is a profound challenge to the clinician’s skill and the patient’s resilience. It requires a meticulous balance of aggressive technical intervention and compassionate, holistic care. By understanding the pathophysiology through the lens of Harrison’s and the diagnostic rigor of French’s Index, we can navigate the complexities of the cold-injured heart and the metabolic shifts of the hypothermic state.
Always remember that our analysis is consultative; the ultimate safety of the patient depends on the hands-on assessment of the physician at the bedside. In our quest for healing, we must respect both the power of advanced technology and the subtle wisdom of natural recovery, always adhering to the sacred vow of doing no harm. Through warmth, patience, and a deep understanding of the human metabolic fire, we can bridge the gap between the chill of exposure and the light of recovery.