Description
Comprehensive clinical analysis and modern strategies for the management of peripheral arterial disease: From pathophysiological mechanisms to integrative therapy
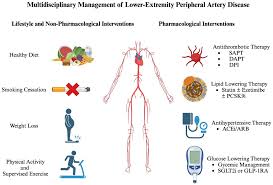
Peripheral arterial disease (PAD) is a broad clinical condition defined by progressive narrowing (stenosis) or complete obstruction (occlusion) of the aorta and its noncardiac branches supplying the lower extremities. As a critical component of systemic atherosclerosis, PAD is not simply an isolated circulatory disorder in the legs but a powerful predictor of generalized vascular involvement, including coronary artery disease and cerebrovascular pathology. Current understanding of the disease, as reflected in the 2024 American College of Cardiology (ACC) and American Heart Association (AHA) guidelines, emphasizes the need for a multidisciplinary approach that combines precise diagnosis, aggressive risk factor modification, and innovative pharmacological and revascularization strategies.
Definition and etiological spectrum of pathology
Peripheral arterial disease encompasses a group of disorders that compromise blood flow to the extremities, with atherosclerosis being the leading etiological cause in the vast majority of cases (over 90% in patients over 40 years of age). The pathological process is characterized by the formation of atherosclerotic plaques in the intima of large and medium-sized arteries, leading to progressive narrowing of the vascular lumen and disruption of the nutritional balance of tissues distal to the lesion site.
Despite the dominant role of atherosclerosis, the clinician must also consider nonatherosclerotic causes of arterial obstruction, which often require a specific diagnostic and therapeutic approach. These alternative etiologies include:
- Thromboembolism: Acute occlusion arising from cardiac sources (atrial fibrillation) or aneurysms.
- Vasculitis: Such as thromboangiitis obliterans (Buerger’s disease), affecting mainly young smokers.
- Fibromuscular dysplasia: A non-inflammatory, non-atherosclerotic disease of the vascular wall.
- Anatomical syndromes: Popliteal entrapment syndrome or adventitial cysts.
- Trauma and radiation exposure: Leading to intimal fibrosis or dissection.
Epidemiology and global socio-economic impact
PAH is a global disease affecting over 237 million people worldwide, with approximately 6.5 million diagnosed in the United States alone. Epidemiological data reveal a strong correlation between the prevalence of the disease and age. While the prevalence in the population under 60 years of age is around 3%, in individuals over 75 years of age it increases to over 20%.
| Demographic group / Region | Prevalence of PAB (%) | Key associated factors |
| General population (>40 years) | 10 – 15% | Age, Smoking |
| Diabetes and smoking (50-69 years) | 29% | Microvascular involvement |
| People over 75 years old | >20% | Isolated systolic hypertension |
| African American population | 2 times higher than whites | Genetics, Social Determinants |
| Global scale (total) | 237 million people | Urbanization, Diabetes pandemic |
The prognosis for patients with PAD is grave, with mortality closely related to the severity of limb ischemia. Patients with intermittent claudication have a 5-year survival rate of 70-85%, while in those with chronic limb-threatening ischemia (CLTI), the 1-year mortality rate reaches a staggering 25%. Most of these patients die not from limb complications but from myocardial infarction or stroke, highlighting the role of PAD as a systemic “red flag” for cardiovascular risk.
Pathology classification and staging
The classification of PAH has undergone significant evolution, moving from purely symptomatic descriptors to complex systems incorporating hemodynamic and anatomical data.
Classical systems: Fontaine and Rutherford
These systems are traditionally used to categorize the severity of ischemia based on clinical manifestations:
- Fontaine classification:
- Stage I: Asymptomatic.
- Stage IIa: Mild claudication (distance walked > 200 m).
- Stage IIb: Moderate to severe claudication (< 200 m).
- Stage III: Ischemic pain at rest.
- Stage IV: Ulcers or gangrene.
- Rutherford Classification: Divides patients into 4 grades and 7 categories (from 0 – asymptomatic to 6 – severe tissue loss).
Modern Classification: The WIfI System (2024)
The most current amputation risk assessment tool recommended by the new ACC/AHA guidelines is the WIfI (Wound, Ischemia, and foot Infection) system . It assesses three critical dimensions, each on a scale of 0 to 3:
- Wound (W): The severity of the ulcer or gangrene is assessed.
- Ischemia (Ischemia – I): Based on ankle pressure, toe pressure (TBI), or transcutaneous partial pressure of oxygen ($TcPO_2$).
- Foot Infection (fI): The presence and spread of the infectious process is assessed.
The combined score allows the physician to determine the patient’s clinical stage (from 1 to 4), which directly correlates with the likelihood of limb salvage and the benefit of urgent revascularization.
Pathophysiology: Hemodynamic and cellular mechanisms
The pathophysiology of PAD is a complex process involving both mechanical obstruction and metabolic dysfunction of skeletal muscle and endothelial degradation.
Atherosclerotic process and vascular architecture
Atherosclerotic lesions are preferentially localized at sites of increased turbulence and altered shear stress, such as arterial branching sites. The most common locations include:
- Aorto-iliac segment (30% of patients).
- Femoro-popliteal segment (80–90% of patients) – especially in the Hunter canal (adductor canal).
- Distal (tibio-peroneal) segment (40–50% of patients), typically in diabetic patients.
Metabolic Mish-Mash and “Ischemic Debt”
Under normal conditions, blood flow to lower limb muscles increases significantly during exercise. Hemodynamically significant stenosis (usually >50% diameter narrowing) prevents this increase. When the metabolic demands of the exercising muscle exceed the supply, lactate and other metabolites accumulate, which stimulate sensory nerve endings, causing pain.
As the disease progresses, compensatory collateral circulation develops. However, collaterals have higher resistance than native arteries, which keeps perfusion pressure low. In severe ischemia (CLTI), microvascular dysfunction and edema are observed, which further impairs oxygen diffusion to the tissues. Interestingly, ischemic pain in these patients often acquires a neuropathic character due to chronic damage to the peripheral nerves (vasa nervorum).
Clinical manifestation and diagnostic phenotypes
The clinical spectrum of PAD is extremely wide – from completely asymptomatic patients to conditions of threatening gangrene.
Intermittent Claudication
The classic symptom is described as muscle pain, stiffness, or a feeling of heaviness that occurs when walking a certain distance and disappears within 2 to 10 minutes of rest. It is important to note that the pain is always localized distal to the level of obstruction:
- Buttock and thigh pain: Aortoiliac disease.
- Calf pain: Femoro-popliteal disease.
- Foot pain: Tibial disease.
Atypical symptoms and asymptomatic profile
Less than half of patients have typical claudication. Many report atypical leg pain, fatigue, or limited mobility, which are often mistaken for signs of aging or arthritis. However, asymptomatic patients carry the same high risk of cardiovascular events, which warrants screening in at-risk groups.
Chronic limb-threatening ischemia (CLTI)
It is characterized by pain at rest that is typically worse at night when the leg is in a horizontal position. Patients often sleep with the leg elevated to use gravity to improve perfusion. Objective findings include nonhealing ulcers (usually on the toes or heel) and focal gangrene.
Acute limb ischemia (ALI)
This is a vascular emergency, manifested by the “6 P’s” syndrome:
- Pain – sudden and severe.
- Pallor – the skin becomes deathly white.
- Pulselessness – distal to occlusion.
- Poikilothermia (Cold) – the limb adopts the temperature of the environment.
- Paresthesia – numbness.
- Paralysis – inability to move.
Diagnosis and diagnostic criteria
The diagnostic process for PAD requires consistent application of clinical and instrumental methods.
Ankle-Brachial Index (ABI) – The Gold Standard
The ABI is the first and most important step in diagnosis. It is calculated as the ratio between the highest systolic pressure in the ankle and the highest in the arm.
| ABI value | Clinical interpretation |
| 1.00 – 1.40 | Normal state |
| 0.91 – 0.99 | Borderline (requires stress test with load) |
| $\le$ 0.90 | Diagnostic for PAB |
| < 0.50 | Severe ischemia (high risk of limb loss) |
| > 1.40 | Non-compressible arteries (calcinosis of the media) |
In patients with ABI > 1.40 (often in diabetes and CKD), measurement of the Toe-Brachial Index (TBI) is mandatory , as the arteries of the fingers rarely calcify. A TBI $\le$ 0.70 confirms the diagnosis.
Physical Examination: Key Findings
A careful examination may reveal:
- Weakened or absent pulsations of the femoral artery, popliteal artery, posterior tibial artery, and dorsalis pedis artery.
- Presence of vascular bruits over the abdominal aorta, iliac or femoral arteries.
- Buerger’s test: Raising the leg 45° results in rapid pallor, and when lowered, delayed, intense redness (dependent rubor) occurs.
- Muscle atrophy, hair loss, thickened nails, and cyanotic, cold skin.
Laboratory tests and biomarkers
In addition to the standard lipid profile, blood sugar, and creatinine, new research points to the importance of specific inflammatory markers:
- hs-CRP (high-sensitivity C-reactive protein): Elevated levels are an independent predictor of PAD progression and risk of heart attack.
- Cystatin C and $\beta$2-Microglobulin: These proteins correlate more strongly with ABI than traditional risk factors and may serve as early markers of vascular damage.
- Homocysteine: Hyperhomocysteinemia doubles the risk of developing peripheral atherosclerosis.
Instrumental and imaging studies
- Doppler sonography (Duplex Ultrasound): First line of imaging. Allows assessment of blood flow velocity and localization of stenoses by measuring PSV (peak systolic velocity). The typical triphasic waveform changes to biphasic or monophasic distal to the obstruction.
- CT Angiography (CTA): Provides a detailed 3D map of the arterial tree. Excellent for planning operations, but limited in severe calcification (“blooming effect”) and requires iodine contrast.
- MR Angiography (MRA): Offers high resolution without ionizing radiation. Non-contrast protocols are valuable in patients with renal failure.
- Angiography (DSA): Remains the “gold standard”, but due to its invasiveness is used primarily during interventional procedures.
Differential diagnosis
Correct recognition of PAH requires exclusion of a number of conditions with similar clinical presentations.
Neurogenic Claudication (Spinal Stenosis)
This is the most common differential diagnostic difficulty. In spinal stenosis, the pain is often relieved by bending forward (the “shopping cart” position) or sitting down, while in PAH, simply standing still is sufficient.
Venous claudication
It occurs in severe venous insufficiency. The pain is described as “cracking” or stretching and is relieved by elevating the legs, which would worsen the pain in arterial insufficiency.
Other conditions:
- Hip/Knee Osteoarthritis: Pain is associated with movement of the joint and is often worst with the first steps in the morning (“moving phenomenon”).
- Peripheral neuropathy: The pain is burning, often present at rest, and has a “stocking” distribution, with no direct relationship to physical exertion.
Therapy: Pharmacotherapeutic goals and strategies
Treatment of PAD is directed towards two main goals: preventing fatal cardiovascular events (MACE) and improving functional capacity of the limb (MALE).
Non-pharmacological and holistic therapy
- Smoking cessation: The most effective measure to improve prognosis. Requires a combination of pharmacology (nicotine replacement therapy, Varenicline) and behavioral support.
- Structured Exercise Training (SET): Recommended for all patients with claudication. The program involves a minimum of 30–45 minutes of treadmill walking, 3 times a week, for at least 12 weeks. The goal is for the patient to walk until moderate pain occurs, then rest and repeat the cycle.
- Diet and Lifestyle: The Mediterranean diet, rich in omega-3 fatty acids, improves endothelial function and reduces systemic inflammation.
Classical pharmacotherapy: Drugs and dosages
- Antiplatelet and antithrombotic therapy
- Aspirin: 75 – 100 mg daily as monotherapy.
- Clopidogrel: 75 mg daily. In the CAPRIE study, it showed better efficacy than aspirin in patients with PAD.
- Combination therapy (COMPASS): The most advanced strategy involves rivaroxaban 2.5 mg twice daily plus aspirin 100 mg once daily . This combination significantly reduces the risk of major cardiovascular events and amputations in high-risk patients.
- Lipid-lowering therapy
All patients with PAD should take high-intensity statins (Atorvastatin 80 mg or Rosuvastatin 20-40 mg). The goal is to reduce LDL-cholesterol by $\ge$ 50% and reach levels below 1.8 mmol/L (70 mg/dL), and in very high risk – below 1.4 mmol/L (55 mg/dL).
- Antihypertensive therapy
The goal is blood pressure < 130/80 mmHg. First-line treatment is ACE inhibitors (e.g. Ramipril) , which, in addition to lowering blood pressure, also have a direct vasoprotective effect.
- Claudication therapy
- Cilostazol: Phosphodiesterase-III inhibitor.
- Dosage: 100 mg twice daily.
- Effect: Improves distance traveled by 40-60%.
- Critical contraindication: Absolutely contraindicated in patients with any degree of heart failure due to risk of fatal arrhythmias.
- Pentoxifylline: 400 mg three times daily. Considered second-line due to weaker evidence of efficacy.
Role of Integrative Medicine: Ginkgo Biloba and Chelation Therapy
extract (EGb 761) is the best-studied herbal remedy. At a dose of 240 mg daily , it improves blood rheology and may increase pain-free walking distance. However, the evidence is weaker than that of cilostazol, and ginkgo should be considered as an adjuvant therapy.
L-Carnitine and Propionyl-L-Carnitine: Improve muscle metabolism and are being studied for increasing exercise capacity.
Potential negative interactions
The integration of phytotherapy with classical medicine poses risks that the doctor should be well aware of.
Risk of bleeding
Ginkgo biloba, garlic, ginger, and turmeric have mild antiplatelet properties. Combining them with potent anticoagulants such as Rivaroxaban or antiplatelet agents such as Clopidogrel may unpredictably increase the risk of severe bleeding. It is recommended to stop taking ginkgo at least 2 weeks before elective surgery.
CYP450 Interactions
- St. John’s wort: Induces CYP3A4, which may reduce blood levels of statins and rivaroxaban, making therapy ineffective.
- Grapefruit juice: Inhibits the metabolism of statins, which sharply increases the risk of myopathy and rhabdomyolysis.
- Omeprazole: May reduce the activation of Clopidogrel. If gastroprotection is needed, Pantoprazole is preferred.
Pharmacokinetic considerations
In acute conditions and the need for rapid clearance of drugs (e.g. in nursing mothers), the 3.3 half-life rule should be applied. Complete elimination of a given drug is achieved after a time equal to its plasma half-life multiplied by 3.3 .
Conclusion and guidelines for clinical practice
Peripheral arterial disease is a dynamic and multifaceted disease that requires a “vigilant” clinical approach. The modern physician must see beyond the leg pain and recognize the systemic risk that the patient carries. The key to success lies in early diagnosis through ABI, strict control of risk factors and the implementation of new antithrombotic regimens (COMPASS). Combining these measures with structured physical activity and informed use of integrative methods can significantly improve the quality of life and reduce mortality in this severe pathology.