Description
The Harmony of Healing: A Comprehensive Clinical Treatise on Urticaria and Angio-oedema
In the sacred pursuit of medical knowledge, one must perceive the human body not merely as a collection of symptoms, but as a living tapestry where the internal and external worlds meet. Urticaria and angio-oedema represent one of the most visible manifestations of this intersection—a sudden disruption of the skin’s tranquility that reflects a deeper, often complex immunological dialogue. To understand these conditions is to understand the body’s innate defensive mechanisms, which, in their zeal to protect, may sometimes disturb the very balance they seek to maintain. Guided by the principle of Primum non nocere, this treatise aims to bridge the gap between high-level molecular pathophysiology and the empathetic care required to restore a patient to a state of equilibrium.
Definition and the Nature of the Pathology
Urticaria is a mast cell-driven disease characterized by the transient appearance of wheals, angio-oedema, or both. A wheal is defined by three essential clinical features: a central swelling of variable size, almost always surrounded by a reflex erythema (the flare); a pruritic or sometimes burning sensation; and an evanescent nature, with the skin typically returning to its normal appearance within 1 to 24 hours.
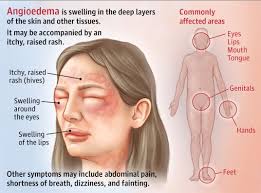
Angio-oedema, while sharing a similar pathophysiological origin with urticaria, involves the deeper layers of the dermis and the subcutaneous or submucosal tissues. It presents as a sudden, pronounced, erythematous or skin-colored swelling. Unlike the wheals of urticaria, angio-oedema is often associated with pain or tingling rather than intense itching, and it resolves more slowly, sometimes taking up to 72 hours for complete resolution. Approximately 40% of patients suffer from both manifestations simultaneously, while 10% may experience angio-oedema in isolation.
Epidemiology and the Global Burden of Disease
The prevalence of urticaria is a testament to its status as a universal human experience. Global data suggests that approximately 20% of the population will encounter at least one episode of acute urticaria during their lifetime. While many of these episodes are fleeting, a significant portion of the population transitions into a chronic state, which imposes a profound burden on the quality of life, affecting physical comfort, psychological well-being, and professional performance.
As of 2024 and 2025, epidemiological trends indicate a rising incidence of chronic spontaneous urticaria (CSU), particularly in urbanized healthcare systems. In the United States, current estimates place the number of diagnosed CSU cases at approximately 885,000, with annual healthcare costs exceeding $200 million.
| Epidemiological Metric | Observation / Value | Source |
| Lifetime Prevalence (Acute) | ~20% of the global population | |
| Point Prevalence (Chronic) | ~0.7% to 1.0% | |
| Gender Predisposition | 2:1 Female-to-Male ratio (Adults) | |
| Peak Age of Incidence | Third to fifth decades (20–40 years) | |
| Remission Rate (1 Year) | ~17% for CSU | |
| Remission Rate (5 Years) | ~71% for CSU |
A landmark international study presented at the 2025 EAACI Congress emphasized that CSU is often not an isolated dermatological event but is frequently linked with systemic comorbidities, including diabetes mellitus, thyroid disorders, and psychiatric conditions like anxiety and panic attacks. This underscores the need for a holistic diagnostic approach that looks beyond the skin’s surface.
Classification: The Temporal and Inducible Spectrum
To categorize urticaria is to understand its rhythm. The primary classification is based on duration, which serves as a critical diagnostic and prognostic marker.
Acute Urticaria
Acute urticaria is defined by the presence of wheals or angio-oedema for a duration of less than six weeks. These episodes are frequently self-limiting and are often triggered by identifiable external factors such as upper respiratory viral infections (especially in children), medications (e.g., NSAIDs, antibiotics), or IgE-mediated food allergies.
Chronic Urticaria
When symptoms recur for more than six weeks, the condition is classified as chronic. This category is further divided into:
- Chronic Spontaneous Urticaria (CSU): Wheals and/or angio-oedema occur without an identifiable external trigger.
- Chronic Inducible Urticaria (CIndU): Symptoms are consistently triggered by a specific physical or environmental stimulus.
The diversity of inducible urticarias reveals the body’s sensitivity to its surroundings:
- Symptomatic Dermographism: Whealing induced by mechanical shearing or stroking of the skin.
- Cold Urticaria: Triggered by cold air, water, or objects.
- Delayed Pressure Urticaria: Swelling that appears hours after sustained pressure, such as from tight clothing or tool usage.
- Solar Urticaria: Induced by exposure to specific wavelengths of light.
- Cholinergic Urticaria: Small wheals triggered by an increase in core body temperature (e.g., exercise, hot baths).
- Aquagenic Urticaria: Triggered by contact with water, regardless of its temperature.
Pathophysiology: The Molecular Dance of Mast Cells
The “Golden Standard” for understanding the cellular mechanisms of urticaria remains Harrison’s Principles of Internal Medicine, which describes a complex interplay of immunological signaling and vascular response. At the heart of this process is the mast cell, a sentinel of the immune system residing in the perivascular spaces of the dermis.
The IgE-Mediated Signaling Pathway
The activation of mast cells typically begins with the cross-linking of the high-affinity FcϵRI receptors on their surface. These receptors consist of an α chain for IgE binding, a β chain, and two γ chains that facilitate signal transduction. When an allergen or auto-antibody cross-links IgE molecules bound to these receptors, a signaling cascade is initiated:
- Kinase Recruitment: The Src family-related tyrosine kinase, Lyn, transphosphorylates the ITAMs of the β and γ
- Syk Activation: This leads to the recruitment and activation of Syk tyrosine kinase.
- Phospholipase Cascade: Activated PLCγ cleaves membrane phospholipids into IP3 and DAG.
- Calcium Mobilization: IP3 triggers the release of intracellular calcium, which is the decisive signal for degranulation.
Degranulation and Mediator Release
Once activated, mast cells release a potent cocktail of mediators:
- Preformed Mediators: Histamine, tryptase, and chymase. Histamine acts on H1 receptors in the skin to cause vasodilation, increased vascular permeability, and the characteristic pruritus.
- Newly Synthesized Mediators: Prostaglandin D2 and leukotrienes (LTC4,LTD4,LTE4). These sustain the inflammatory response and contribute to the prolonged swelling seen in angio-oedema.
The Autoimmune Component
In approximately 40% to 60% of patients with CSU, the “trigger” is internal—an autoimmune response. This may involve Type I autoimmunity (IgE against autoallergens like thyroid peroxidase) or Type IIb autoimmunity (IgG autoantibodies against FcϵRI or IgE itself). This understanding explains why CSU is often associated with other autoimmune conditions, particularly Hashimoto’s thyroiditis.
The Kinin Pathway in Angio-oedema
While histamine is the driver in most cases, a distinct pathway involving the kinin system is responsible for non-pruritic angio-oedema, such as Hereditary Angioedema (HAE). In HAE, the deficiency of C1-esterase inhibitor leads to the uncontrolled generation of bradykinin, a powerful vasodilator that acts on B2 receptors to cause profound tissue swelling without the associated whealing or itching of histamine-mediated reactions.
Clinical Manifestation: The Language of the Skin
The clinical diagnosis of urticaria is based on the recognition of its characteristic lesions. Patients often present with a history of recurrent, itchy eruptions that seem to migrate across different body regions—from the scalp to the soles of the feet.
Characteristics of Urticarial Wheals
Wheals are well-circumscribed, raised, and often have a blanched (pale) center with a red, serpiginous border. They are intensely pruritic, and this itching is typically most severe at night. A critical observation is the lack of residual scarring or bruising; if a lesion leaves a mark after resolving, one must suspect underlying vasculitis.
Manifestations of Angio-oedema
Angio-oedema is marked by asymmetric, dramatic swelling that is often more painful or burning than itchy. It commonly affects:
- The Face: Periorbital and perioral regions.
- The Extremities: Hands and feet.
- The Upper Respiratory Tract: Swelling of the tongue, uvula, and larynx, which can lead to life-threatening airway obstruction.
- The Gastrointestinal Tract: Edema of the bowel wall can cause intense abdominal colic, nausea, and vomiting, often mimicking a surgical emergency.
Diagnostics: A Methodical Exploration
In the wisdom of medical practice, the most powerful diagnostic tool remains a thorough history and physical examination. Extensive laboratory investigations are generally not indicated for acute urticaria unless a specific allergen is strongly suspected.
Diagnostic Criteria and Physical Examination
The physical examination should involve a search for triggers. Eliciting dermographism—the appearance of a linear wheal after firm pressure—can often be performed in the clinic to confirm a physical subtype. For chronic cases, clinicians use the Urticaria Activity Score (UAS7), a patient-reported tool that tracks the number of wheals and the severity of itch over seven days to assess disease control.
Laboratory Investigations
When symptoms persist or systemic involvement is suspected, a systematic laboratory workup is necessary:
- Initial Screen: CBC with differential and inflammatory markers (ESR/CRP) to rule out systemic inflammation or infection.
- Allergy Evaluation: Skin prick tests or serum specific IgE (RAST) if Type I triggers like food or insect venom are suspected.
- Autoimmune and Metabolic Profile: TSH and thyroid autoantibodies (anti-TPO, anti-TG) are essential given the strong link between CSU and autoimmune thyroiditis.
- Complement System: If angio-oedema occurs without urticaria, measuring serum C4 levels is a vital screening step. A low C4 level suggests HAE, which is then confirmed by measuring the level and functional activity of C1-esterase inhibitor.
- Biopsy: Indicated if lesions last >24 hours, are painful rather than itchy, or leave residual purpura, to evaluate for urticarial vasculitis.
Instrumental and Imaging Diagnostics
Imaging is rarely required for typical urticaria but is lifesaving in cases of suspected visceral angio-oedema:
- Computed Tomography (CT): For patients presenting with “acute abdomen,” a CT scan with contrast can reveal segmental thickening of the small bowel wall, mucosal enhancement, and the presence of ascites.
- Point-of-Care Ultrasound (POCUS): In the emergency department, POCUS can rapidly identify bowel wall edema (measured as >5mm) and free intra-abdominal fluid, facilitating an early diagnosis of HAE-related abdominal attacks.
Differential Diagnosis: The French’s Index Approach
To provide clarity in the face of complex clinical signs, we apply the analytical approach of French’s Index of Differential Diagnosis, categorizing conditions by their probability and severity.
Most Probable (Common Clinical Presentations)
- Acute and Chronic Spontaneous Urticaria: The primary diagnosis characterized by evanescent, pruritic wheals.
- Atopic Dermatitis: Distinguished by chronic, eczematous lesions that are typically lichenified and lack the transient nature of wheals.
- Insect Bites (Papular Urticaria): Lesions persist for days and often have a central punctum.
Less Probable but Clinically Distinct
- Allergic Contact Dermatitis: The eruption is localized to the area of allergen contact and involves vesiculation and scaling.
- Erythema Multiforme: Presents with characteristic “target” or “iris” lesions and is often triggered by infections like Herpes Simplex.
- Bullous Pemphigoid (Prodromal Stage): In older adults, intense pruritus and urticarial plaques may precede the development of bullae by weeks.
Rare but Severe (Life-Threatening or Systemic)
- Anaphylaxis: Acute urticaria and angio-oedema accompanied by systemic symptoms (hypotension, wheezing, GI distress). This is a medical emergency requiring immediate epinephrine.
- Hereditary Angioedema (HAE): Recurrent, non-pruritic swelling of the face, airway, or bowel wall. Absence of urticaria is a key diagnostic clue.
- Urticarial Vasculitis: Lesions last >24 hours, are painful, and biopsy shows necrotizing vasculitis. Often associated with systemic lupus erythematosus.
- Schnitzler Syndrome: Chronic urticaria combined with monoclonal IgM gammopathy and systemic inflammatory symptoms.
| Differential Diagnosis | Key Distinguishing Feature | Probable Pathology | Source |
| Evanescent Wheals (<24h) | Intensely Pruritic | True Urticaria | |
| Persistent Plaques (>24h) | Painful / Bruising | Urticarial Vasculitis | |
| Facial/Bowel Swelling | No Wheals / No Itch | Bradykinin-mediated (HAE) | |
| Eczematous Lesions | Chronic / Excoriated | Atopic Dermatitis | |
| Target Lesions | Central Dusky Zone | Erythema Multiforme |
Therapy: A Journey Toward Balance
The ultimate goal of therapy is complete symptom relief until the disease reaches spontaneous remission. The treatment plan must be both scientifically rigorous and compassionate.
Step-by-Step Pharmacotherapy (EAACI/GA2LEN Standards)
The 2022 international guidelines recommend a tiered pharmacological approach :
- First-Line: Standard-dosed modern, second-generation H1-antihistamines (e.g., Bilastine 20 mg, Cetirizine 10 mg, Desloratadine 5 mg, or Fexofenadine 180 mg). First-generation agents (e.g., Diphenhydramine) should be avoided due to their significant CNS side effects and interference with REM sleep.
- Second-Line: If control is not achieved within 2–4 weeks, increase the dose of the same antihistamine up to fourfold (e.g., Cetirizine 20 mg twice daily). Updosing a single agent is preferred over mixing multiple types.
- Third-Line: Add-on Omalizumab (anti-IgE) at 300 mg every four weeks. This is highly effective for patients refractory to high-dose antihistamines.
- Fourth-Line: Add-on Ciclosporin A (3.5–5 mg/kg/day) for severe, refractory cases. This requires close monitoring of blood pressure and renal function.
Non-Pharmacological and Holistic Interventions
Restoring health requires more than just suppression of symptoms; it requires a return to lifestyle harmony :
- Pseudoallergen-Free Diet: Avoiding artificial colors, preservatives, and natural salicylates can significantly reduce symptom severity in many CSU patients.
- Nutritional Support:
- Vitamin D: Supplementation is recommended if serum levels are low, as it modulates immune function in chronic urticaria.
- Vitamin C: High doses (1000–3000 mg) act as a natural antihistamine and mast cell stabilizer.
- Quercetin: A flavonoid that inhibits the release of histamine and inflammatory cytokines from mast cells.
- Mind-Body Balance: Stress is a potent trigger for flares. Techniques such as progressive muscle relaxation, meditation, and adequate sleep are foundational to health planning.
Management of Hereditary Angioedema
Treatment of HAE focuses on the bradykinin pathway rather than antihistamines. Acute attacks are treated with C1-inhibitor concentrates, Icatibant (B2 receptor antagonist), or Ecallantide. Prophylaxis includes androgens (which stimulate C1-INH production) or monoclonal antibodies like Lanadelumab.
Critical Precautions: Herb-Drug and Supplement Interactions
A holistic approach demands vigilance regarding the interactions between classic pharmacology and natural remedies. The principle of Primum non nocere is especially relevant here.
Quercetin Interactions
While Quercetin is a powerful mast cell stabilizer, it can alter the metabolism of several essential drugs by interacting with OATP pumps and CYP450 enzymes :
- Anticoagulants: Quercetin can enhance the effect of Warfarin, increasing the risk of bleeding.
- Immunosuppressants: It may increase levels of Cyclosporine, potentially leading to toxicity.
- Cardiovascular Drugs: It can increase the concentration of certain statins (Pravastatin, Rosuvastatin), increasing the risk of muscle toxicity.
Licorice Root (Glycyrrhiza glabra) Interactions
Licorice is used in traditional medicine for its anti-inflammatory properties, but its glycyrrhizin content carries significant risks :
- Potassium Depletion: Licorice increases potassium excretion. Combined with diuretics (Furosemide) or corticosteroids, it can lead to severe hypokalemia, causing cardiac arrhythmias.
- Hypertension: Licorice causes sodium and water retention, which can counteract the effects of antihypertensive medications like ACE inhibitors and beta-blockers.
- Digoxin Toxicity: Hypokalemia induced by licorice dramatically increases the heart’s sensitivity to Digoxin, which can be fatal.
Vitamin C and D Precautions
High-dose Vitamin C can interfere with the absorption of certain medications and should be taken at least two hours apart from other drugs. Vitamin D, while generally safe, should be monitored to avoid hypercalcemia, particularly in patients on thiazide diuretics.
Conclusion: The Path Toward Equilibrium
Urticaria and angio-oedema are not merely skin diseases; they are profound expressions of the body’s internal state and its interaction with the environment. By embracing both the precision of modern immunology and the wisdom of a holistic, patient-centered approach, we can guide our patients from the chaos of a flare toward the tranquility of remission.
Medicine is the art of restoring harmony. As practitioners, we must remain ever-watchful for the serious signs of systemic disease, gentle in our communication with those who suffer, and rigorous in our scientific application. Let every treatment plan be a “health plan” co-authored with the patient, built on continuity, follow-up, and the unwavering pursuit of well-being.
Clinical Disclaimer: This comprehensive analysis is intended for medical professionals and students as a consultative guide. Urticaria and angio-oedema can be signs of life-threatening anaphylaxis or severe systemic disease. All patients must be evaluated by a physical physician for definitive diagnosis and treatment. In cases of respiratory distress or cardiovascular collapse, emergency protocols (epinephrine administration) must be initiated immediately..