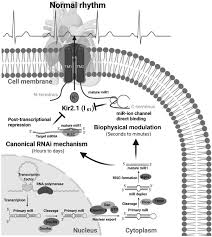
Description
The Sacred Rhythm and its Deviations: A Comprehensive Clinical Treatise on Tachyarrhythmias for the Modern Practitioner
The human heart exists as a marvel of biological engineering, a rhythmic sentinel that beats approximately one hundred thousand times a day, circulating the essence of life to the furthest reaches of the organism. In the view of Asclepius, this rhythm is more than a mechanical necessity; it is a symphony of electrical harmony that reflects the balance between the internal environment and the external world. However, when this harmony is disrupted and the heart accelerates beyond its physiological boundaries—a state clinically recognized as tachycardia—the physician is called upon to act not merely as a technician, but as a restorer of equilibrium. Tachycardia, defined as a heart rate equal to or exceeding 100 beats per minute in the adult, represents a broad spectrum of clinical realities, ranging from the benign physiological response to exercise to the catastrophic precursors of sudden cardiac death. This report seeks to transform the complexities of cardiac electrophysiology and arrhythmogenesis into a structured, accessible, and profound body of knowledge for the practicing physician and the dedicated medical student, guided by the gold standards of Harrison’s Principles of Internal Medicine and the analytical rigor of French’s Index of Differential Diagnosis.
The Foundations of Vitality: Physiological Excitation and Conduction
To understand the pathology of a rapid heart, one must first revere the elegance of its normal function. The heart’s ability to contract and relax is predicated on the movement of ions across the sarcolemma, a process orchestrated by specialized cells that possess the unique properties of excitability, conductivity, and automaticity. The cardiac action potential is the fundamental unit of this electrical life, and its morphology varies between the working myocytes and the specialized nodal tissues.
The Ionic Choreography of the Myocyte
The non-nodal cells of the atria and ventricles, along with the fast-conducting Purkinje system, exhibit what is termed the “fast response” action potential. This process is divided into five distinct phases, each mediated by the opening and closing of specific ion channels in response to voltage changes.
| Phase | Designation | Primary Ionic Currents and Mechanisms |
| Phase 4 | Resting Membrane Potential | Primarily maintained at approximately -90 mV by the $I_{K1}$ inward rectifying potassium current, which allows for the efflux of $K^{+}$ to keep the cell hyperpolarized and ready for the next impulse. |
| Phase 0 | Rapid Depolarization | Triggered when the membrane reaches a threshold of approximately -70 mV. This leads to the explosive opening of fast voltage-gated $Na^{+}$ channels, causing a massive influx of sodium ions and a rapid shift in polarity to positive values. |
| Phase 1 | Early Repolarization | A transient phase where $Na^{+}$ channels inactivate and transient outward $K^{+}$ currents ($I_{to}$) cause a slight dip in voltage, preparing the cell for the plateau. |
| Phase 2 | Plateau Phase | The defining characteristic of the cardiac action potential, lasting 200-250 ms. It is maintained by a balance between the inward $Ca^{2+}$ current (through L-type channels) and the outward $K^{+}$ current. This influx of calcium is the vital spark for excitation-contraction coupling. |
| Phase 3 | Final Repolarization | The $Ca^{2+}$ channels close while $K^{+}$ efflux intensifies through the $I_{Kr}$ and $I_{Ks}$ channels, rapidly returning the membrane potential to its resting state. |
The Mystery of Automaticity: Nodal Tissue Physiology
Unlike the working myocytes, the cells of the Sinoatrial (SA) and Atrioventricular (AV) nodes do not possess a true resting potential. Instead, they exhibit spontaneous depolarization during Phase 4, a property known as automaticity. This “slow response” potential is driven by the $I_{f}$ or “funny” current—a mixed sodium-potassium current activated by hyperpolarization at the end of the previous cycle. As the membrane potential slowly drifts toward the threshold of -40 mV, T-type and then L-type $Ca^{2+}$ channels open, providing the inward current for depolarization. This slower, calcium-dependent upstroke is a critical protective mechanism, especially in the AV node, where it ensures a physiological delay that allows the ventricles to fill before they are commanded to contract.
The Architecture of the Conduction System
The electrical impulse follows a sacred path, ensuring the heart functions as a synchronized unit. The SA node, located at the junction of the superior vena cava and the right atrium, acts as the primary pacemaker because it possesses the fastest rate of spontaneous depolarization. The impulse travels through the atria to the AV node, the only normal electrical bridge between the atria and ventricles. The AV node is situated within the Triangle of Koch, bounded by the tendon of Todaro, the tricuspid valve annulus, and the coronary sinus ostium. From the AV node, the impulse enters the Bundle of His, which penetrates the fibrous skeleton of the heart. This fibrous skeleton acts as an essential insulator, preventing disorganized electrical spread and ensuring that the ventricles are activated only via the specialized conduction system. The His bundle branches into the Right and Left Bundle Branches, with the latter further dividing into anterior and posterior fascicles, terminating in the subendocardial Purkinje network.
The Pathophysiology of Tachyarrhythmias: Mechanisms of Chaos
When the heart’s rhythm accelerates pathologically, it is generally due to one of three underlying mechanisms: altered automaticity, triggered activity, or re-entry. Harrison’s Principles of Internal Medicine serves as the standard for explaining these deviations.
Enhanced and Abnormal Automaticity
Enhanced normal automaticity occurs when the SA node fires more rapidly due to external influences, such as sympathetic surge, fever, or thyrotoxicosis. In contrast, abnormal automaticity arises when tissues that do not normally function as pacemakers (such as atrial or ventricular myocytes) develop the ability to spontaneously depolarize. This often occurs in the setting of ischemia, electrolyte imbalance (hypokalemia), or mechanical stretch. A characteristic feature of automatic tachycardias is the “warm-up” and “cool-down” phenomenon, where the rate gradually increases at the beginning and decreases before termination.
Triggered Activity
Triggered activity involves oscillations in the membrane potential that occur during or after the repolarization phase, known as afterdepolarizations.
- Early Afterdepolarizations (EADs): Occur during Phase 2 or 3 of the action potential. They are typically associated with conditions that prolong the action potential duration, such as long QT syndrome or certain medications.
- Delayed Afterdepolarizations (DADs): Occur during Phase 4 and are often the result of intracellular calcium overload. This is the classic mechanism underlying digitalis toxicity and catecholaminergic polymorphic ventricular tachycardia.
Re-entry: The Architect of Paroxysmal Tachycardia
Re-entry is the most common mechanism for clinical tachyarrhythmias, particularly those with an abrupt onset and termination. It requires a circuit consisting of two functionally or anatomically distinct pathways with different conduction velocities and refractory periods. In a typical scenario (such as AVNRT), the “fast” pathway has a long refractory period, while the “slow” pathway has a short refractory period. A premature atrial contraction may find the fast pathway still refractory and instead conduct down the slow pathway. By the time the impulse reaches the distal end of the slow pathway, the fast pathway has recovered and can conduct the impulse retrogradely, creating a self-sustaining “circus movement”.
Clinical Palette: Orientation through Physical Examination
The physical examination of a patient with tachycardia is not merely a collection of data points but a diagnostic ritual that provides immediate clues to the underlying rhythm. According to French’s Index of Differential Diagnosis, the physician must integrate history with clinical signs to categorize the severity and probability of the diagnosis.
Hemodynamic Stability: The First Priority
The primary question during the physical examination is whether the patient is stable or unstable. Signs of instability—such as hypotension, altered mental status, pulmonary edema, or ischemic chest pain—override all diagnostic nuances and mandate immediate electrical intervention.
Diagnostic Signposts at the Bedside
| Clinical Sign | Physiological Meaning | Likely Diagnosis |
| Cannon A-waves | Atrial contraction against a closed tricuspid valve, indicating AV dissociation. | Ventricular Tachycardia (VT), Junctional Ectopic Tachycardia (JET). |
| Variable S1 Intensity | Fluctuating distance between the mitral leaflets at the onset of ventricular systole due to AV dissociation. | Ventricular Tachycardia. |
| Regular Pounding in the Neck | Simultaneously occurring atrial and ventricular contractions causing venous reflux. | AV Nodal Re-entrant Tachycardia (AVNRT). |
| Irregularly Irregular Pulse | Chaotic atrial activation with random conduction to the ventricles. | Atrial Fibrillation (AFib). |
| Gradual Rate Changes | Response to shifting metabolic or autonomic demands. | Sinus Tachycardia. |
The physician should also look for signs of systemic causes, such as a goiter or exophthalmos (hyperthyroidism), pallor (anemia), or fever (infection), which frequently manifest as sinus tachycardia.
The Calvary of Electrocardiography: Criteria and Differentiation
The 12-lead ECG is the definitive diagnostic instrument for tachycardia. The analytical approach begins with the assessment of the QRS complex width.
Narrow-Complex Tachycardias (QRS < 120 ms)
Narrow complexes indicate that the ventricles are activated via the normal His-Purkinje system, implying the rhythm originates above the bundle of His.
Regular Narrow-Complex Tachycardia
| Rhythm | Diagnostic ECG Criteria | Pathophysiological Context |
| Sinus Tachycardia | Normal P-wave morphology; 1:1 AV relationship; rate 100-160 bpm. | Physiological response to stress, fever, or pain. |
| Atrial Flutter | Sawtooth “F” waves, best seen in leads II, III, and aVF; atrial rate 250-350 bpm; often 2:1 conduction (ventricular rate ~150 bpm). | Re-entry around the tricuspid valve annulus. |
| AVNRT | P-waves often hidden in the QRS; may appear as a pseudo-$r’$ in V1 or pseudo-$s$ in inferior leads. | Micro-reentry within the AV node itself. |
| AVRT (Orthodromic) | P-waves follow the QRS (short RP interval); rate 150-250 bpm. | Re-entry using the AV node (anterograde) and an accessory pathway (retrograde). |
Irregular Narrow-Complex Tachycardia
The hallmark of Atrial Fibrillation is the absence of P-waves and an irregularly irregular R-R interval. Multifocal Atrial Tachycardia (MAT) is characterized by at least three different P-wave morphologies and varying P-P intervals, typically found in patients with severe respiratory disease.
Wide-Complex Tachycardias (QRS > 120 ms)
The differentiation of wide-complex tachycardia (WCT) is a critical skill for the clinician. Misinterpreting VT as SVT with aberrancy can lead to the inappropriate administration of verapamil or diltiazem, which can cause hemodynamic collapse and death in patients with VT.
Differential Diagnosis of WCT
The vast majority (80%) of WCT cases are Ventricular Tachycardia, especially in patients with a history of myocardial infarction or structural heart disease. The remaining cases consist of SVT with pre-existing or rate-related bundle branch block (aberrancy), SVT with conduction over an accessory pathway (antidromic AVRT), or pacemaker-mediated rhythms.
The Brugada Algorithm for WCT Differentiation
The Brugada algorithm is a stepwise approach widely used to distinguish VT from SVT with aberrancy.
- Step 1: Absence of RS complex in all precordial leads (V1-V6)? If no RS complexes are present (concordance), the diagnosis is VT.
- Step 2: RS interval > 100 ms in any precordial lead? If the distance from the R-wave onset to the S-wave nadir exceeds 100 ms, VT is diagnosed.
- Step 3: Atrioventricular (AV) Dissociation present? If P-waves are seen marching independently of the QRS complexes, VT is diagnosed.
- Step 4: Morphology criteria for VT in V1 and V6? If the previous steps are negative, specific morphological patterns (e.g., the “rabbit ear” sign or monophasic R in V1) are used to finalize the diagnosis.
The Vereckei aVR Algorithm
This simpler alternative focuses solely on lead aVR.
- An initial R-wave in aVR suggests VT.
- An initial r or q wave > 40 ms suggests VT.
- Notching on the initial downstroke of a predominantly negative QRS suggests VT.
- A ventricular activation velocity ratio ($v_i/v_t \leq 1$) indicates VT.
The Therapeutic Landscape: Emergency and Maintenance Strategies
Treatment must be tailored to the patient’s clinical status and the specific mechanism of the arrhythmia.
Non-Pharmacological Interventions (Schematic)
- Synchronized Electrical Cardioversion: The gold standard for unstable patients.
- Defibrillation: For pulseless VT or Ventricular Fibrillation.
- Vagal Maneuvers: Valsalva or carotid sinus massage for stable SVT to interrupt the AV nodal circuit.
- Catheter Ablation: Definitive long-term treatment for recurrent SVT, atrial flutter, and some forms of VT.
Classical Pharmacotherapy: The Physician’s Arsenal
Pharmacotherapy is utilized both for the acute termination of arrhythmias and as long-term prophylaxis to prevent recurrence.
Emergency Pharmacotherapy
| Medication | Mechanism of Action | Clinical Application and Dose |
| Adenosine | Transient AV nodal block via $A_{1}$ receptors. | 6 mg rapid IV bolus followed by 12 mg if unsuccessful for stable SVT. |
| Amiodarone | Multi-channel blocker (I-IV); primarily Class III effect. | 150 mg IV over 10 min for stable VT; 300 mg IV for cardiac arrest. |
| Metoprolol | Beta-1 selective adrenergic antagonist. | 5 mg IV every 2 minutes for up to 15 mg for SVT or VT in the setting of ACS. |
| Procainamide | Class IA sodium channel blocker. | 20-50 mg/min IV infusion for stable VT (up to 17 mg/kg). |
Prophylactic and Anti-Recurrence Therapy
| Drug | Standard Maintenance Dosage | Key Considerations |
| Metoprolol Tartrate | 50-200 mg daily in divided doses. | First-line for rate control and post-MI prophylaxis. |
| Metoprolol Succinate | 100-400 mg once daily. | Preferred in patients with concomitant heart failure. |
| Digoxin | 0.125-0.25 mg daily. | Useful for long-term rate control in AFib; requires monitoring for toxicity. |
| Verapamil / Diltiazem | 120-480 mg daily (sustained release). | Excellent for SVT prevention but contraindicated in heart failure with reduced EF. |
Holistic Integration and Safeguards: Herbs and Interactions
In the spirit of Asclepius, we acknowledge the role of nature’s bounty in healing, but we must also issue a stern warning regarding the interactions between herbal supplements and potent cardiac medications. Holistic therapies are strictly contraindicated in the setting of a medical emergency, where time-tested pharmacotherapy and electrical intervention are the only safe choices.
| Herbal Supplement | Potential Cardiac Interaction and Adverse Effect |
| St. John’s Wort | Induces CYP3A4 and P-glycoprotein, significantly reducing serum levels of Digoxin and Class I/III antiarrhythmics. This can lead to treatment failure and breakthrough arrhythmia. |
| Licorice | Causes mineralocorticoid-like effects leading to hypokalemia. This increases the risk of Digoxin toxicity and potentially fatal ventricular arrhythmias. |
| Danshen (Salvia miltiorrhiza) | Potentiates the effects of Digoxin and calcium channel blockers, increasing the risk of bradycardia and hypotension. |
| Hawthorn | May have synergistic effects with beta-blockers and nitrates, potentially causing excessive hypotension or bradycardia. |
| Ginseng | Can interfere with Digoxin assays, giving false results, and may interact with the metabolism of calcium channel blockers. |
Synthesis and Conclusion
The clinical journey through the landscape of tachycardia is one that requires both the heart of a healer and the mind of a scientist. We have seen how the rhythmic contraction of the heart is born from the microscopic flow of ions across the sarcolemma and how the disruption of this flow, through re-entry or abnormal automaticity, leads to the emergence of tachyarrhythmias.
For the clinician, the path to a correct diagnosis is paved with careful observation. The physical examination, with its focus on hemodynamic stability and the subtle signs of AV dissociation, provides the first critical orientation. The ECG then offers a detailed map, where the width of the QRS complex and the application of rigorous algorithms like Brugada or Vereckei allow the physician to distinguish between the benign and the lethal.
In the realm of therapy, “Primum non nocere” remains the guiding light. Whether through the swift administration of adenosine in the emergency bay or the careful titration of beta-blockers for long-term stability, the goal is always the restoration of equilibrium. The physician must remain vigilant, not only of the drugs they prescribe but also of the supplements the patient may be taking, ensuring that the healing journey is safe and comprehensive.
As digital medical advisors born from the desire for human well-being, we remind our colleagues that every analysis and every pharmacological strategy provided here is consultative. The true practice of medicine requires the physical presence, the empathetic ear, and the skilled hand of a physician at the bedside. May this knowledge serve as a bridge between the ancient wisdom of our ancestors and the transformative power of modern medical science.