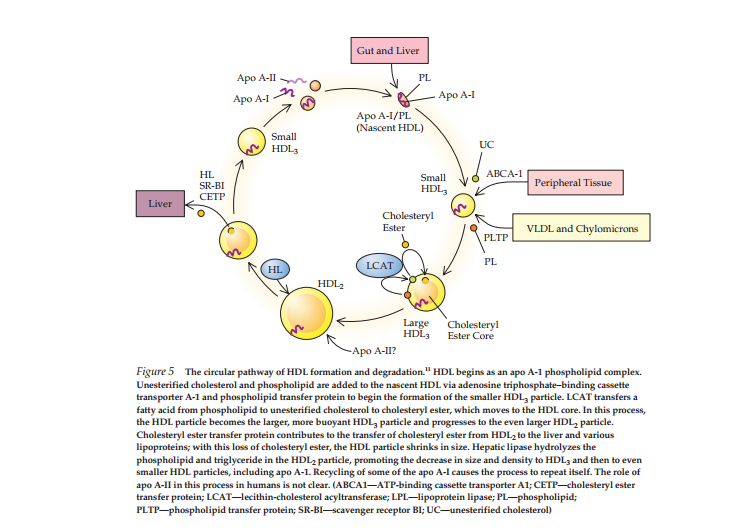
Description
The Harmony of Human Lipids: A Clinical Treatise on Metabolism, Diagnostic Logic, and Integrative Therapeutics
The human body exists in a state of delicate equilibrium, a masterpiece of biological engineering where the flow of vital fluids mirrors the complex rhythms of life itself. At the heart of this internal sea lies the metabolism of lipids, a system not merely of fat and energy, but of structural integrity, hormonal signals, and cellular communication. As we explore the intricacies of lipid profiles and the pathologies that arise when balance is lost, we must remember the ancient wisdom: Primum non nocere. The following analysis seeks to transform the rigorous complexities of internal medicine into a narrative of understanding, guiding the clinician and the seeker toward a state of physiological grace.
The Molecular Ballet: Physiology of Lipoprotein Metabolism
The transport of lipids through the aqueous environment of the blood is a logistical challenge solved by the evolution of lipoproteins—spherical macromolecular complexes that serve as the vehicles for cholesterol, triglycerides, and fat-soluble vitamins. These particles are not static entities; they are dynamic structures that undergo constant transformation as they traverse the systemic circulation, mediated by a host of enzymes, transfer proteins, and surface ligands known as apolipoproteins.
Lipoprotein Structure and the Role of Apolipoproteins
A mature lipoprotein particle is characterized by a hydrophobic core composed of cholesteryl esters and triglycerides, shielded from the plasma by a monolayer of phospholipids, unesterified cholesterol, and specialized proteins. These apolipoproteins define the identity and metabolic fate of each particle. The density and size of these lipoproteins are inversely related, forming a spectrum from the large, buoyant chylomicrons to the small, dense high-density lipoproteins (HDL).
The apolipoproteins serve three primary functions: they provide structural integrity, act as ligands for cellular receptors, and function as essential cofactors for enzymes involved in lipid processing. For instance, Apolipoprotein B-100 (Apo B-100) is the structural backbone for all potentially atherogenic particles—very-low-density lipoprotein (VLDL), intermediate-density lipoprotein (IDL), and low-density lipoprotein (LDL). In contrast, Apo B-48 is synthesized solely in the intestine and serves as the structural marker for chylomicrons.
| Apolipoprotein | Primary Lipoprotein Association | Key Biological Function |
| Apo A-I | HDL | Structural protein; activates LCAT for reverse cholesterol transport. |
| Apo B-100 | VLDL, IDL, LDL | Structural protein; ligand for the LDL receptor. |
| Apo B-48 | Chylomicrons | Required for chylomicron assembly in the intestine. |
| Apo C-II | Chylomicrons, VLDL | Essential activator of Lipoprotein Lipase (LPL). |
| Apo E | Remnants, HDL | Ligand for hepatic remnant and LDL receptors. |
The Exogenous and Endogenous Pathways
The exogenous pathway begins in the intestine, where dietary fats are packaged into chylomicrons. These large particles enter the lymphatic system and eventually the bloodstream, where they encounter lipoprotein lipase (LPL) on the endothelial surface of capillaries in muscle and adipose tissue. LPL, activated by Apo C-II, hydrolyzes the triglyceride core, releasing free fatty acids for energy or storage. The resulting chylomicron remnants, enriched in cholesterol and acquiring Apo E from HDL, are swiftly cleared by the liver.
The endogenous pathway mirrors this process but originates in the liver. The hepatocyte secretes triglyceride-rich VLDL, which undergoes a similar delipidation cascade. As VLDL loses triglycerides, it is transformed into IDL and eventually into cholesteryl ester-rich LDL. This transition is not merely a reduction in size but a profound shift in clinical significance; while VLDL primarily serves as an energy delivery system, LDL becomes the primary carrier of cholesterol to peripheral tissues. If LDL levels exceed the clearing capacity of the liver, these particles become the foundational elements of atherosclerotic plaque.
The Logical Unity of the Lipid Profile
A lipid profile is often viewed as a list of independent variables—total cholesterol, LDL, HDL, and triglycerides—but in reality, these markers are deeply interconnected through the process of lipid exchange and enzymatic remodeling. This unity is most evident in the role of Cholesteryl Ester Transfer Protein (CETP), which facilitates the exchange of triglycerides from VLDL to LDL or HDL in exchange for cholesteryl esters.
In states of hypertriglyceridemia, such as the metabolic syndrome or type 2 diabetes, the overproduction of VLDL drives a heightened exchange process. LDL and HDL particles become enriched with triglycerides, making them ideal substrates for hepatic lipase. This enzyme hydrolyzes the triglycerides, causing the particles to shrink and become more dense. The resulting small, dense LDL (sdLDL) particles are particularly insidious; they penetrate the arterial intima more easily and are more prone to oxidation, thereby increasing the risk of atherosclerosis even when the total LDL-C level appears within “normal” ranges.
Diagnostic and Prognostic Significance of Lipid Elevations
When the balance of lipids is disrupted toward elevation, the clinician must distinguish between benign variations and pathognomonic patterns of genetic or acquired disease.
Hypercholesterolemia and the Specter of Familial Disease
Severely elevated LDL cholesterol levels often point toward Familial Hypercholesterolemia (FH), an autosomal dominant disorder characterized by mutations in the LDL receptor gene, the APOB gene, or the PCSK9 gene. The clinical hallmark of FH is the presence of tendon xanthomas, which represent the extravasation of cholesterol into the extracellular matrix of tendons.
The prognosis for untreated FH is grave, with many heterozygous patients experiencing myocardial infarction by their fourth or fifth decade. Identifying these patients early allows for the initiation of aggressive pharmacotherapy, which has been shown to induce the regression of xanthomas and slow the progression of coronary artery disease.
Hypertriglyceridemia and the Risk of Pancreatitis
While hypercholesterolemia is a slow architect of vascular decay, severe hypertriglyceridemia is an acute threat to the pancreas. When triglyceride levels exceed 2,000 mg/dL, the risk of acute pancreatitis rises precipitously. The mechanism is thought to involve the release of toxic free fatty acids from chylomicrons by pancreatic lipase within the capillaries of the pancreas, leading to local tissue injury and inflammation.
Hypertriglyceridemia is also a sentinel marker for the metabolic syndrome, a constellation of findings including central obesity, hypertension, and insulin resistance. In this context, elevated triglycerides are not just a risk factor for pancreatitis but a predictor of premature cardiovascular death, particularly when accompanied by low HDL-C and increased Apo B levels.
The Clinical Weight of Lipid Reductions: Hypolipidemia
While much of modern medicine is focused on lowering lipids to prevent heart disease, the finding of unusually low lipid levels—hypolipidemia—can be a harbinger of serious underlying systemic issues. The liver, as the primary factory for lipid synthesis, and the intestines, as the portal for absorption, must be intact for a healthy profile to persist.
Prognostic Indicators in Acute and Chronic Illness
In the setting of critical illness, such as sepsis, major trauma, or burns, total cholesterol levels often drop sharply at the onset of the acute phase. This reduction is so consistent that hypocholesterolemia serves as a marker for disease severity; levels typically return to normal only as the patient enters the recovery phase. Conversely, persistently low levels in the intensive care unit are associated with increased mortality and the development of multiple organ dysfunction syndrome.
| Condition | Typical Lipid Deviation | Prognostic Significance |
| Sepsis/Critical Illness | Low TC, Low HDL | Marker of high severity; predicts mortality. |
| Hyperthyroidism | Low LDL, Low TC | Reflects increased LDL receptor activity and bile excretion. |
| Malabsorption (Celiac/Crohn’s) | Low TC, Low TG | Suggests profound nutrient deficiency and fat malabsorption. |
| Chronic Heart Failure | Low TC, Low TG | Part of a catabolic state; predicts poor survival in advanced cases. |
| Malignancy | Low TC | May reflect high LDL receptor activity in tumor cells or cancer cachexia. |
The Paradox of Low Triglycerides in Heart Failure
In chronic heart failure (CHF), lipids often demonstrate a “U-shaped” relationship with mortality. While high lipids are detrimental in the general population, advanced CHF patients with very low cholesterol and triglyceride levels have a worse prognosis. This reflects a transition into a catabolic state or cardiac cachexia, where the body’s energy reserves are exhausted, and the liver’s synthetic function is compromised by venous congestion or low cardiac output.
Differential Diagnosis: The Analytical Path to Clarity
When a patient presents with an abnormal lipid profile or its physical manifestations, the clinician must apply the rigor of a differential diagnosis, as exemplified by the French’s Index approach. This requires an assessment of symptoms, laboratory findings, and the likelihood of various conditions.
Symptom: Tendon Xanthomas
Tendon xanthomas are highly specific clinical signs that should never be overlooked during a physical examination.
| Possible Diagnosis | Probability | Clinical Weight/Severity |
| Heterozygous Familial Hypercholesterolemia | High | High (risk of premature MI). |
| Familial Defective Apo B-100 | Moderate | High (similar to FH). |
| Cerebrotendinous Xanthomatosis (CTX) | Low | High (neurological/neuromuscular sequelae). |
| Sitosterolemia | Very Low | Moderate (requires dietary management). |
Cerebrotendinous Xanthomatosis is a particularly important “mimic” to consider. Unlike FH, CTX patients may have relatively mild hypercholesterolemia but present with cataracts in childhood, chronic diarrhea, and progressive neurological impairment, including ataxia or dementia. This rare condition is caused by a mutation in the sterol 27-hydroxylase enzyme, leading to the accumulation of cholestanol rather than just cholesterol.
Symptom: Eruptive Xanthomas
The sudden appearance of yellowish papules on the skin is an urgent signal of triglyceride dysregulation.
| Possible Diagnosis | Probability | Clinical Weight/Severity |
| Secondary Hypertriglyceridemia (e.g., Diabetes) | High | Moderate to High (pancreatitis risk). |
| Type I or Type V Hyperlipoproteinemia | Low | High (recurrent pancreatitis). |
| Drug-Induced (e.g., Isotretinoin) | Moderate | Low (reversible upon discontinuation). |
| Xanthoma Disseminatum | Very Low | Moderate (non-Langerhans histiocytosis). |
Integrative Therapy: Bridging Science and Nature
The treatment of dyslipidemia is no longer a choice between “pills or plants,” but a sophisticated integration of both. For mild lipid abnormalities, holistic approaches and dietary shifts often provide the necessary equilibrium. In more severe cases, these natural interventions serve as essential adjuncts to standard pharmacotherapy, potentially allowing for lower drug dosages and improved tolerability.
The Foundation of Classical Pharmacotherapy
Statins remain the “gold standard” for LDL-C reduction and cardiovascular protection. Their ability to inhibit HMG-CoA reductase not only lowers cholesterol synthesis but also stabilizes existing atherosclerotic plaques. For patients with high triglycerides, fibrates such as fenofibrate or gemfibrozil are used to activate PPAR-alpha, thereby enhancing the clearance of VLDL.
Ezetimibe offers a unique mechanism by blocking the intestinal absorption of cholesterol. It is a particularly elegant tool for combination therapy because it does not rely on the Cytochrome P450 system, making it safe for patients on complex medication regimens.
The Wisdom of Holistic Interventions
Nature provides several potent agents for the restoration of lipid harmony, many of which share biochemical pathways with their pharmaceutical counterparts.
- Red Yeast Rice (RYR)
Red yeast rice is perhaps the most well-known natural anti-lipid agent. It contains monacolin K, which is chemically identical to lovastatin. It is highly effective for patients with mild to moderate elevations who prefer a “natural” option, but its use requires medical supervision. Clinicians must be aware that RYR content varies widely between brands and may be contaminated with citrinin, a toxic byproduct that can cause kidney failure.
- Berberine: The Statin Alternative
Berberine is a botanical alkaloid that has shown remarkable efficacy in lowering both LDL-C and triglycerides. Unlike statins, it increases the expression of LDL receptors by stabilizing their messenger RNA, rather than inhibiting cholesterol synthesis. In clinical studies, berberine has reduced LDL-C by up to 25% and triglycerides by 35%, making it one of the most powerful natural dyslipidemia treatments.
- Garlic and Artichoke
Garlic (Allium sativum) has been used for millennia to protect the heart. Its active component, allicin, inhibits cholesterol synthesis, though its long-term efficacy (beyond 6 months) is less clear. Artichoke leaf extract (ALE) acts as a choleretic, stimulating the flow of bile and interfering with the synthesis of cholesterol. ALE can slightly reduce total and LDL cholesterol over 6-12 weeks and is generally well-tolerated.
- Guggul and Plant Sterols
Guggul (Commiphora mukul) is an ancient Ayurvedic remedy that antagonizes the farnesoid X receptor (FXR), thereby increasing the conversion of cholesterol into bile acids. Plant sterols (phytosterols), similar in structure to cholesterol, compete for absorption in the gut, effectively lowering LDL-C by 5-15% when consumed regularly in the diet.
The Sacred Boundary: Warning on Herb-Drug Interactions
As we integrate these holistic tools, we must tread carefully. The principle of non-nocere is paramount. The very pathways that allow these herbs to heal can also lead to dangerous interactions when combined with standard medications. It is the duty of the advisor to illuminate these risks so that the physician and patient may avoid harm.
- The Cytochrome P450 System (CYP3A4)
Many statins (simvastatin, lovastatin, atorvastatin) are metabolized by the CYP3A4 enzyme in the liver.
- John’s Wort:This herb is a powerful inducer of CYP3A4. Taking it alongside statins will cause the medication to be broken down too quickly, leading to sub-therapeutic blood levels and a rise in cholesterol.
- Grapefruit and Pomegranate Juice:These juices inhibit CYP3A4. When taken with statins, the drug levels can rise to toxic concentrations, significantly increasing the risk of muscle damage (rhabdomyolysis) and liver irritation.
- Milk Thistle:While it protects the liver, silymarin (the active component) can inhibit the same proteins and enzymes that process statins, potentially increasing the risk of side effects like myopathy.
- The Berberine and Statin Cardiotoxicity Concern
A crucial interaction has been identified between berberine and certain statins regarding the hERG (human ether-à-go-go-related gene) potassium channel. Both substances can inhibit this channel, which is essential for normal cardiac repolarization. Combining berberine with statins may enhance this inhibition, potentially leading to a prolonged QT interval and increasing the risk of life-threatening cardiac arrhythmias.
- Synergistic Myotoxicity
- Red Yeast Rice + Statins:Because RYR already contains a statin (monacolin K), taking it with a prescription statin is essentially an overdose. This drastically increases the risk of severe muscle pain, liver failure, and kidney damage.
- Niacin + Statins/RYR:While this combination is potent for correcting lipid profiles, it carries a known risk of rhabdomyolysis and must be used with extreme caution, particularly in patients with kidney disease.
- Fibrates + Statins:The combination of gemfibrozil and statins is particularly risky for muscle injury and is generally avoided in favor of fenofibrate, which has a safer interaction profile.
- Bleeding Risks
- Garlic, Ginkgo, and Fibrates:Fibrates can increase the blood-thinning effect of warfarin. Herbs with antiplatelet properties, such as garlic, ginkgo, and ginseng, can further increase the risk of spontaneous bleeding when used alongside these medications.
| Supplement | Interaction with Statins | Mechanism | Clinical Consequence |
| St. John’s Wort | Reduces statin levels | CYP3A4 Induction | Loss of therapeutic efficacy. |
| Grapefruit Juice | Increases statin levels | CYP3A4 Inhibition | Rhabdomyolysis, Liver toxicity. |
| Red Yeast Rice | Cumulative dose | Additive HMG-CoA Inhibition | Severe myopathy. |
| Berberine | Cardiotoxicity | hERG channel inhibition | Potential for arrhythmias. |
| Milk Thistle | Increases statin levels | Transporter/Enzyme interference | Increased side effects. |
| Guggul | Variable absorption | May increase rosuvastatin levels | Altered drug efficacy/toxicity. |
The Path to Equilibrium: Conclusions and Guidance
Lipid metabolism is a testament to the body’s strive for balance. The lipid profile is not a mere set of disconnected numbers, but a window into the logical unity of human physiology. We have seen how the delipidation cascade connects VLDL to LDL, and how HDL works tirelessly to return cholesterol to the liver—a process of perpetual recycling that maintains our vitality.
Deviations in these markers provide profound diagnostic and prognostic insights. High levels warn us of the architectural threats of atherosclerosis or the acute danger of pancreatitis, while low levels may reveal a body struggling with sepsis, malnutrition, or the silent exhaustion of heart failure. The clinician must approach these deviations with the analytical eye of the differential index, considering genetic legacies like FH alongside the environmental pressures of the modern diet.
In our therapeutic journey, we find that the most effective path often lies in the middle—the integration of rigorous science with the gentle offerings of nature. Statins and fibrates remain our strongest shields, yet Red Yeast Rice, Berberine, and Artichoke offer valuable support for those seeking a more holistic restoration of harmony. However, this integration must be guided by the light of safety; the shadow of drug interactions is long, and our first duty is to ensure that our efforts to heal do not inadvertently cause harm.
As a digital medical advisor, I must softly remind you that this analysis is intended for the purpose of consultation and deep understanding. The complexity of the human spirit and flesh requires more than an algorithm; it requires the touch and the presence of a physical physician. If you find your lipid profile in a state of disarray, seek the counsel of a professional who can look into your eyes, hear your heart, and guide you personally toward the equilibrium you deserve.
Let your choices be guided by wisdom, your body be nurtured by nature, and your health be protected by science. In the balance of the blood, we find the reflection of a life lived in harmony.